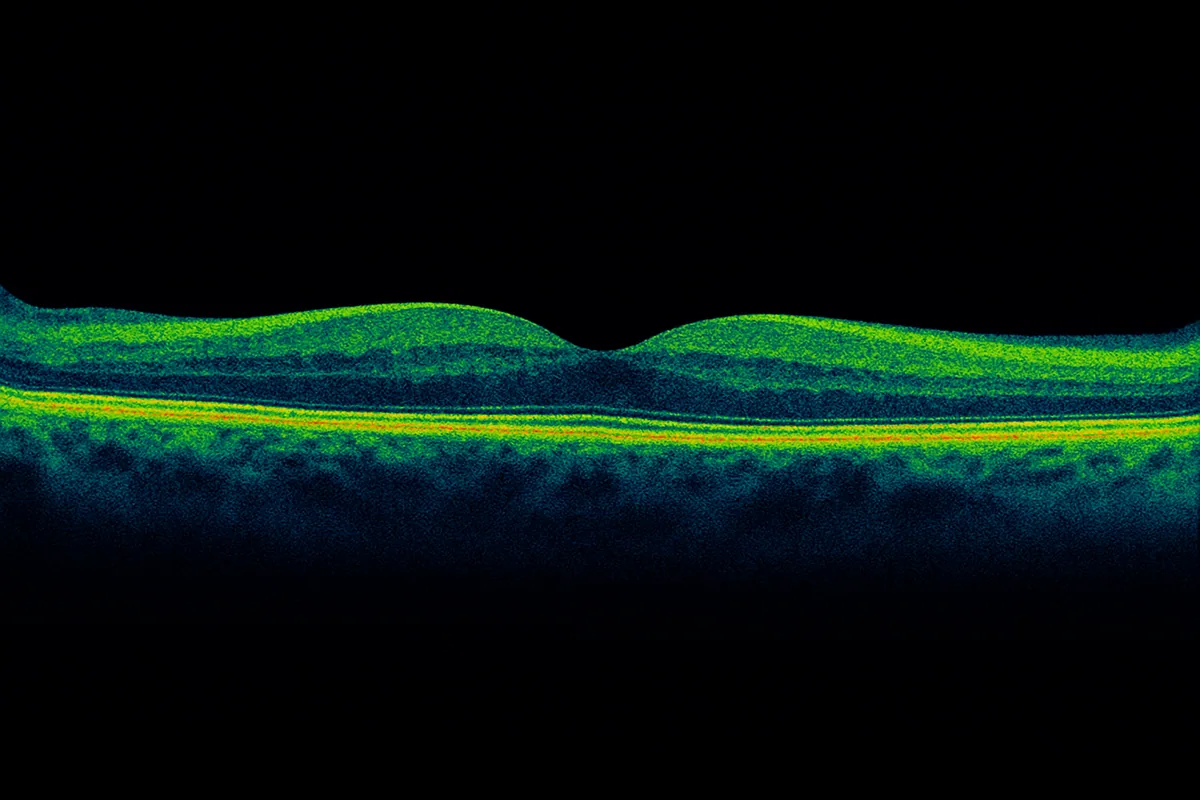
OCT (optical coherence tomography) is a retinal imaging examination that has become essential in ophthalmology. It allows highly precise analysis of the macula – the central area of the retina responsible for fine vision. Dr Julien Gozlan, ophthalmic surgeon in Paris 16, explains what macular OCT involves, when it is indicated, and how the examination is performed.
What is retinal OCT?
OCT (Optical Coherence Tomography) is an imaging examination that produces very thin cross-sections of the retina, similar to a CT scan but using light rather than X-rays. It is completely painless and non-invasive.
The central portion of the retina is called the macula. It is responsible for detailed vision: reading, recognizing faces, driving, and more. On OCT, a normal macula appears as a tissue composed of several well-organized layers stacked on top of one another. At the center, a small depression corresponds to the fovea, the area of sharpest vision.
Anatomical overview: retina, vitreous, and hyaloid
Behind the lens, the interior of the eye is filled with a perfectly transparent gel: the vitreous. This gel is surrounded by a thin membrane called the hyaloid.
At birth and in young adults, the vitreous and hyaloid are firmly attached to the retina at the back of the eye. With age – most commonly after 50 – the hyaloid gradually separates from the retinal surface: this is known as posterior vitreous detachment, a phenomenon that is usually normal and age-related.
OCT allows very precise visualization of the relationship between the retina and the vitreous: it can show whether the vitreous is still attached to the macula, in the process of detaching, or already completely separated.
What is macular OCT used for?
Retinal OCT is indicated whenever a macular condition is suspected or central vision is impaired. It is particularly useful for diagnosing:
- Age-related macular degeneration (AMD): observation of deposits, distortions, and the possible presence of fluid beneath or within the retina
- Macular edema: thickening of the macula, often related to diabetes, retinal vein occlusion, or inflammation; this includes, for example, diabetic macular edema
- Epiretinal membrane: a thin film developing on the surface of the macula that can cause it to pucker
- Vitreomacular traction: areas where the vitreous exerts abnormal pulling on the macula, sometimes in the context of myopic tractional maculopathy
- Macular hole: a round opening in the center of the macula, causing decreased central vision
OCT is also very useful for treatment monitoring, whether involving intravitreal injections or vitreoretinal surgery, by enabling comparison of the macula's appearance over time.
OCT and posterior vitreous detachment
As mentioned above, posterior vitreous detachment is a common occurrence after the age of 50. In the vast majority of cases, it proceeds without complications and requires only simple monitoring.
In rare situations, in the peripheral retina, an abnormally strong adhesion between the hyaloid and the retina can lead to the formation of a retinal tear, which may progress to retinal detachment.
Macular OCT does not replace examination of the peripheral fundus, but it does allow visualization of vitreous traction on the macula, documentation of posterior vitreous detachment, and better understanding of certain symptoms (visual distortions, central blind spot, decreased vision). Depending on the case, it may be supplemented by fluorescein angiography or indocyanine green angiography.
How is an OCT examination performed?
Positioning at the device
The patient sits with their chin on the rest and forehead against the support bar of the device. They fix their gaze on a light point inside the machine. If needed, mydriatic eye drops may be instilled beforehand to dilate the pupil and improve image quality.
Image acquisition
The machine performs several light scans of the macula within seconds. The examination generally lasts a few minutes per eye. There is no contact with the eye: the examination is completely painless.
Results analysis
The images are interpreted by the ophthalmologist in real time on the device screen. The report and images are provided to the patient at the end of the consultation.
A risk-free and highly informative examination
OCT presents no known risk: no radiation, no injection, no pain. It can be repeated as often as necessary to monitor the progression of a retinal disease or the effectiveness of treatment.
The images obtained are immediately analyzed by Dr Julien Gozlan, who interprets them based on your clinical history, visual acuity, and fundus examination findings. The examination is thus part of a comprehensive retinal assessment, whether for diabetic retinopathy, AMD, or another macular condition.
FAQ: frequently asked questions about macular OCT
Is any special preparation required before a macular OCT?
In the vast majority of cases, no preparation is needed: fasting is not required and you can take your usual medications. It is simply recommended that you bring your glasses and, if applicable, let the staff know if you wear contact lenses. In some patients, the doctor may suggest pupil dilation to improve image quality: in that case, it is best to avoid driving immediately after the examination, as your vision will remain blurry for a few hours.
Does OCT replace the fundus examination or angiography?
No, OCT does not replace the fundus examination or angiography: it complements them. OCT shows the architecture of the central retina in detail, layer by layer, whereas the fundus examination explores the entire retina, including the periphery. Angiography, on the other hand, analyzes blood flow and dye leakage. Depending on the condition, the doctor combines these examinations to obtain an overall picture of the situation and tailor the treatment accordingly.
Is OCT covered by national health insurance?
Yes, OCT is covered when performed in the context of a recognized condition (AMD, macular edema, diabetic retinopathy, etc.), according to current reimbursement rules. The remaining out-of-pocket cost depends on your supplementary insurance plan and the practitioner's fee sector. If in doubt, the office staff can clarify the fee conditions before the examination.
Is OCT compatible with pregnancy or a pacemaker?
Yes, OCT is an examination that does not use X-rays, relying instead on a low-intensity light beam. It does not expose you to radiation and does not interact with implanted devices (pacemaker, defibrillator, cochlear implant, etc.). It can therefore be performed on pregnant women and patients with implanted devices, if the doctor considers it useful for retinal monitoring.
What happens if I blink or move during the examination?
A blink or slight movement may simply result in a blurry or incomplete image. In that case, the examiner simply retakes the scan: OCT can be repeated as many times as necessary without any risk to the eye. You will be guided to help you fixate more comfortably on the light target for a few seconds, long enough to obtain clear cross-sections of the macula.
How often should a macular OCT be repeated?
The frequency of OCT examinations depends entirely on the disease being monitored and its stage of progression. In certain active conditions (exudative AMD, macular edema under injection therapy), the examination may be repeated at each consultation to adjust treatment. In more stable situations or for a simple check-up, an occasional OCT may suffice. The schedule is therefore personalized based on your symptoms, treatments, and previous results.
What is the difference between an OCT and an "eye scan" or an MRI?
The expression "eye scan" is often used by patients to refer to OCT, but it is not a CT scan in the radiological sense. OCT does not use X-rays and visualizes only the retina and macular region in detail. CT scans and MRIs, on the other hand, explore the entire eyeball and surrounding structures (orbits, optic nerve, brain) for other types of conditions. These are therefore complementary examinations, indicated in very different contexts.
📍 Macular OCT at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan performs retinal OCT at the Paris – Auteuil Ophthalmology Practice to establish a precise diagnosis of macular diseases and to provide optimal monitoring of your treatment.
Book an AppointmentFurther reading
- Age-related macular degeneration (AMD): causes, symptoms, and treatments.
- Macular epiretinal membrane: symptoms, OCT, and surgical options.
- Intravitreal injections: procedure, indications, and aftercare.
- Vitrectomy: indications and principles of the procedure.
- Retinal detachment: warning signs and management.