Retinal detachment surgery is an ophthalmological emergency: without prompt treatment, vision can be permanently lost. Retinal detachment surgery primarily relies on two techniques: cryopexy with scleral buckling and vitrectomy. Dr Julien Gozlan, ophthalmic surgeon in Paris 16, explains the differences between these procedures, their indications, and postoperative course.
What is a retinal detachment?
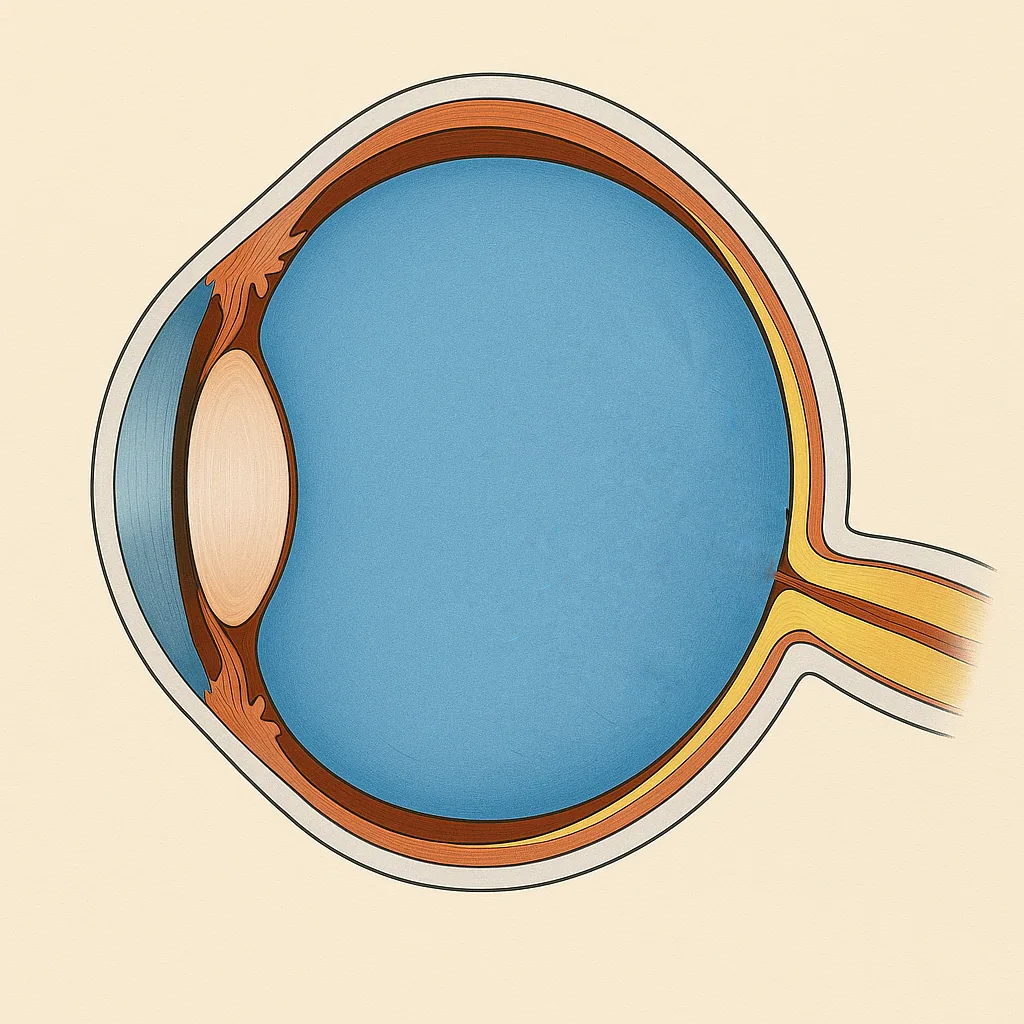
The retina is a thin membrane lining the back of the eye, responsible for converting light into nerve signals. In the case of retinal detachment, this membrane lifts away from its underlying support, much like wallpaper peeling off a wall. Most often, it all begins with a retinal tear through which fluid passes and lifts the retina.
The classic warning signs are:
- the sudden appearance of a large number of floaters;
- flashes of light (photopsia);
- the sensation of a dark curtain or shadow in the visual field;
- a sometimes significant decrease in vision.
If you experience these symptoms, seek emergency care: only retinal detachment surgery can reattach the retina and offer hope of recovering vision.
Key principles of retinal detachment surgery
Regardless of the type of procedure, the objectives are the same:
- seal the causative tear or tears;
- reattach the retina against its underlying support;
- stabilize the situation while healing takes place.
To achieve this, the surgeon can act either from outside the eye with cryopexy and scleral buckling, or from inside with a vitrectomy, or sometimes by combining both techniques.
Preoperative assessment: factors that guide the choice of technique
Before choosing the strategy, the examination determines several decisive factors:
- whether the detachment is macula-on (macula still attached) or macula-off (macula detached);
- the number and location of tears;
- the extent of the detachment and how long-standing it is;
- the presence of traction or proliferative vitreoretinopathy (PVR);
- lens status: phakic (natural crystalline lens) or pseudophakic (intraocular lens implant after cataract surgery);
- the clinical context (high myopia, trauma, prior surgical history).
These criteria explain why no single technique is "better" in absolute terms: the best surgery is the one most suited to the specific configuration of the retinal detachment.
Cryopexy with scleral buckling: acting from the outside
Cryopexy with scleral buckling is a classic technique in retinal detachment surgery. The goal is to push the wall of the eye toward the retina to "plug" the tear from the outside and reduce traction.
In practice, the surgeon:
- locates the retinal tear;
- applies cryotherapy (intense cold) to this area to create a strong adhesion;
- places a silicone band on the sclera (the white outer shell of the eye) that creates an inward indentation.
This approach is often indicated in young, phakic patients with a limited retinal detachment and tears accessible in the periphery. The advantage is that it preserves the vitreous and avoids entering the inside of the eye.
Vitrectomy: treating retinal detachment from the inside
Vitrectomy involves removing the vitreous, the transparent gel that fills the inside of the eye, and then directly treating the tears from within. It is currently the most widely used technique for retinal detachment, particularly in older patients or those who have already undergone cataract surgery.
During the procedure, the surgeon:
- makes micro-incisions in the sclera;
- removes the vitreous and eliminates the traction pulling on the retina;
- treats the tears with laser or cryotherapy;
- fills the eye with a gas or sometimes silicone oil to hold the retina flat against the wall.
Vitrectomy is preferred in cases of complex retinal detachment, extensive forms, recurrences, and cases with PVR or when the patient is pseudophakic.
Gas or silicone oil: why use a tamponade?
In vitrectomy, the surgeon often uses an internal tamponade to hold the retina in place while the treated areas around the tears heal:
- Intraocular gas: it resorbs spontaneously over several weeks. Vision is very blurry at first and gradually improves as the gas diminishes.
- Silicone oil: reserved for certain more complex cases (PVR, recurrence, inability to maintain positioning, etc.). It often requires a second procedure for removal.
When gas is present, air travel and altitude are contraindicated until the gas has completely resorbed, as the bubble can expand and dangerously increase intraocular pressure.
Proliferative vitreoretinopathy (PVR): why it is a risk factor for recurrence
Proliferative vitreoretinopathy (PVR) is one of the main causes of failure or recurrence of retinal detachment. It involves an excessive scarring reaction: cells proliferate and form membranes on the surface of the retina or beneath it, capable of pulling on the tissue.
In practice, PVR can:
- create new traction and reopen a fragile area;
- cause a "rigid" detachment that is more difficult to reattach;
- require more complex procedures (membrane peeling, retinectomy in severe cases);
- increase the need for long-term tamponade, sometimes with silicone oil.
PVR is more common in certain situations: long-standing or very extensive detachment, intravitreal hemorrhage, trauma, recurrences, or inflammation. This explains why some detachments require multiple surgical stages and prolonged follow-up.
Cryopexy with scleral buckling or vitrectomy: how to choose?
The choice of technique depends on the characteristics of the retinal detachment and the patient:
- age and lens status (phakic or pseudophakic);
- number, size, and location of tears;
- extent and duration of the detachment;
- presence or absence of tractional membranes or PVR;
- risk of recurrence and associated factors (high myopia, trauma, prior history).
In a young patient with a limited detachment and a peripheral tear, cryopexy with scleral buckling can be an excellent option. Conversely, for an extensive, long-standing, pseudophakic, or complicated detachment, a vitrectomy often provides better control of traction and recurrence. In some cases, both techniques may be combined.
How is retinal detachment surgery performed?
Preoperative assessment and choice of technique
A full work-up is performed before surgery: OCT, ultrasound if the media are opaque, mapping of the tears. The patient's age, lens status (phakic or pseudophakic), extent of detachment and location of tears guide the choice between cryo-indentation and vitrectomy.
Cryo-indentation (scleral buckling)
The surgeon locates the retinal tear, applies cryotherapy (intense cold) to create a firm scar, then places a silicone band on the sclera that indents the eye wall toward the retina. This technique, preferred in young phakic patients with accessible peripheral tears, preserves the vitreous without entering the eye.
Vitrectomy
The surgeon makes micro-incisions in the sclera, removes the vitreous and relieves traction on the retina, then treats the tears with endolaser or cryotherapy. In cases of extensive proliferative vitreoretinopathy (PVR), a retinectomy allows the rigid retina to be flattened. The cavity is then filled with gas or silicone oil to hold the retina in place.
Immediate postoperative period
After vitrectomy with gas tamponade, strict face-down or lateral positioning is required (depending on tear location), and air travel is contraindicated until the gas is fully absorbed. After scleral buckling or silicone oil tamponade, no positional restriction applies. Close follow-up is required in all cases.
Postoperative course and recovery
After retinal detachment surgery, the eye may be red, sensitive, and vision very blurry at first, especially with gas tamponade. A specific head position may be required for several hours a day over several days (depending on the location of the tears).
Return to activities is gradual: driving, sports, and strenuous exertion are generally postponed. With intraocular gas, air travel and stays at altitude are contraindicated until complete resorption. Close follow-up ensures the retina remains properly reattached.
Visual prognosis: what determines recovery?
The prognosis depends mainly on two factors:
- the status of the macula (macula-on versus macula-off);
- the time to treatment and the complexity of the detachment (PVR, recurrence, extent).
When the macula is still attached (macula-on) and surgery is performed promptly, visual recovery can be excellent. In cases where the macula is detached, vision often improves after reattachment, but recovery may be partial and slower, over several weeks to several months.
FAQ: cryopexy with scleral buckling or vitrectomy for retinal detachment
Is it always an emergency?
Yes, retinal detachment must be treated promptly. The sooner the procedure is performed, the more the risk of detachment progression is limited and the higher the chances of visual recovery, especially if the macula is not yet detached. In practice, an urgent evaluation helps determine the extent, the causative tear or tears, and the best strategy (cryopexy with scleral buckling or vitrectomy).
Which technique gives the best results?
No single technique is systematically superior. The choice depends on very specific criteria: age, lens status (phakic/pseudophakic), location and number of tears, extent of the detachment, presence of intravitreal hemorrhage, and risk of PVR (proliferative vitreoretinopathy). The goal is to achieve a lasting anatomical reattachment with the best functional outcome for your situation.
Why is cryopexy with scleral buckling sometimes recommended for young patients?
In a young phakic patient with a well-identified and accessible peripheral tear, cryopexy with scleral buckling allows treatment of the cause without entering the eye. This notably limits the risk of secondary cataract associated with vitrectomy, while ensuring closure of the tear (cryotherapy) and mechanical support (buckle) to promote healing.
Why is gas placed in the eye after vitrectomy?
After vitrectomy, a gas tamponade is used to press the retina against the inner wall of the eye while the treated areas around the tears heal. Vision is very blurry at first because the bubble occupies a large portion of the vitreous cavity, then it gradually improves as the gas resorbs and is replaced by aqueous humor.
Can you fly after surgery?
Not if there is a gas bubble in the eye. Air travel (and altitude in general) is contraindicated until complete resorption of the gas, as the bubble can expand and dangerously increase intraocular pressure. Your surgeon will specify the duration based on the type of gas used and your postoperative progress.
How long does recovery take?
Recovery depends on the technique (cryopexy with scleral buckling or vitrectomy), the tamponade (gas, silicone oil), and whether the macula was involved. Vision may remain blurry for several weeks, and improvement can continue over several months. If the macula was detached, recovery is often slower and sometimes incomplete, even if the retina is successfully reattached.
Is there a risk of recurrence?
A risk of recurrence exists, especially in complex cases, in the presence of PVR, multiple tears, or retinal fragility (high myopia, trauma, prior history). Postoperative follow-up is essential to detect early any new tear, developing detachment, or complication, so that prompt intervention can be carried out if needed.
When should you seek urgent care after surgery?
You should seek urgent care in case of significant pain, sudden decrease in vision, appearance of a dark curtain, rapid worsening of symptoms, or significant redness associated with light sensitivity. These signs may indicate a complication (ocular hypertension, infection, recurrence) that requires immediate evaluation.
Dr Julien Gozlan, ophthalmologist in Paris 16, evaluates on a case-by-case basis the best strategy for retinal detachment surgery: cryopexy with scleral buckling, vitrectomy, or a combined approach, in order to maximize the chances of success while taking into account your personal situation.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan sees patients at the Paris – Auteuil Ophthalmology Practice for the diagnosis of retinal tears and detachments, and the development of a personalized treatment plan (cryopexy with scleral buckling, vitrectomy, follow-up).
Book an AppointmentFurther reading
- Retinal detachment: symptoms, emergency care, and treatments.
- Vitrectomy: principles of vitreoretinal surgery.
- Macular OCT: the key examination for analyzing the retina.
- Amsler grid: a simple self-monitoring tool for central vision.
- Retinal detachment emergency: act fast : when and how to seek emergency care before surgery.