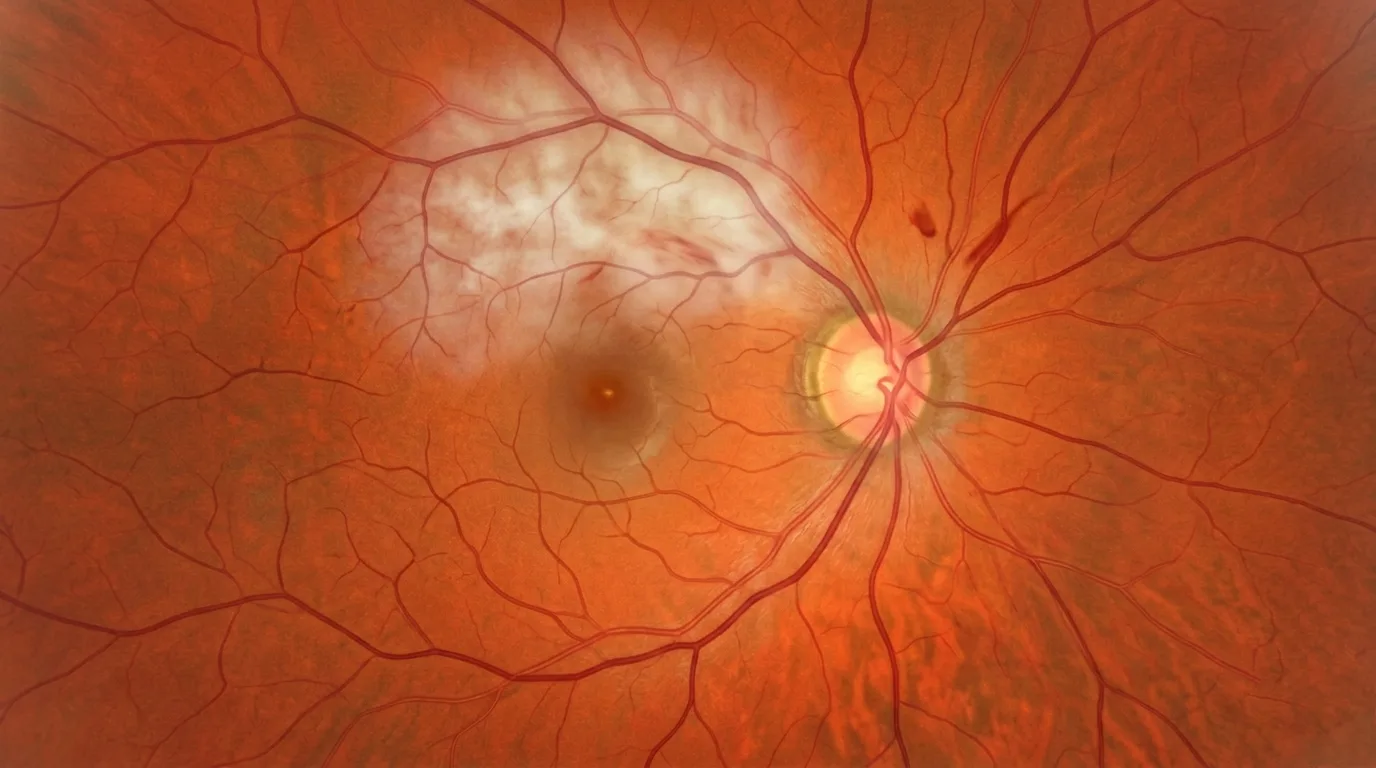
Retinal artery occlusion is an ophthalmological emergency characterized by sudden vision loss, comparable to a stroke of the eye. This rare but serious condition results from the interruption of blood flow in an artery supplying the retina, causing ischemia that can lead to irreversible damage within a few hours. Dr Julien Gozlan, retinal specialist at the Paris – Auteuil Ophthalmology Practice, explains in this article the different forms of retinal artery occlusion, their causes, warning symptoms, diagnostic examinations performed (fundus examination, OCT, OCT angiography), emergency management, visual prognosis, and the critical importance of the associated cardiovascular workup.
What is retinal artery occlusion?
Retinal artery occlusion refers to the blockage of an artery that supplies the retina with oxygenated blood. The retina, a nerve tissue lining the back of the eye, has what is known as terminal vascularization: this means there is no collateral network between the retinal arteries and the choroidal vessels. When an artery becomes blocked, the downstream territory no longer receives blood and undergoes acute ischemia. It is classically considered that damage becomes irreversible beyond 4 hours of non-perfusion, even though the retina has a slightly higher tolerance to ischemia than the brain.
Several forms of retinal artery occlusion are distinguished based on the level of obstruction:
- Central retinal artery occlusion (CRAO): the most common (57% of cases) and the most severe, affecting the entire inner retina.
- Branch retinal artery occlusion (BRAO): accounts for 38% of cases, with ischemia limited to a sector of the retina.
- Cilioretinal artery occlusion: approximately 5% of cases, affecting the interpapillomacular territory.
- Ophthalmic artery occlusion: the most severe form, interrupting both retinal and choroidal circulation.
The incidence of retinal artery occlusions is estimated between 0.5 and 1.5 per 10,000 people per year. In the majority of cases, it involves a male patient (66%) over 60 years of age with cardiovascular risk factors (hypertension, diabetes, hypercholesterolemia, smoking).
Causes and risk factors of retinal artery occlusion
Retinal artery occlusion is most often of embolic origin. A small fragment of material — called an embolus — detaches from a carotid atherosclerotic plaque or a cardiac lesion, migrates through the bloodstream, and obstructs a retinal artery, usually at a bifurcation. Three main types of emboli are distinguished:
- Cholesterol emboli (Hollenhorst plaques): shiny, yellowish, originating from carotid plaques.
- Fibrinoplatelet emboli: grayish, elongated, also arising from atherosclerosis.
- Calcific emboli: whitish, large in size, suggestive of valvular heart disease.
Other causes of retinal artery occlusion include:
- Inflammatory thromboses, notably giant cell arteritis (Horton's disease), which accounts for 1 to 4% of CRAOs and requires emergency corticosteroid therapy.
- Systemic vasculitides: lupus, Behçet's disease, Susac syndrome, Takayasu's disease.
- Carotid dissections, to be suspected in a young patient presenting with neck pain.
- Coagulation disorders (protein C or S deficiency, antiphospholipid syndrome, hyperhomocysteinemia).
- Rare intraocular causes: prepapillary vascular loops, compression from an infectious focus, vascular spasms.
Carotid atherosclerosis is found in 45% of patients with retinal artery occlusion. The presence of retinal emboli is associated in 15 to 25% of cases with areas of silent cerebral ischemia, underscoring the close link between this ocular condition and the risk of stroke.
Symptoms: recognizing retinal artery occlusion
The cardinal symptom of retinal artery occlusion is a sudden, painless, unilateral loss of vision. The patient typically describes a sudden black curtain over one eye, occurring within seconds. Depending on the clinical form:
- CRAO without foveal sparing: vision is profoundly reduced, limited to light perception or "counting fingers." More than 90% of patients have visual acuity equal to or worse than counting fingers.
- CRAO with foveal sparing: if a cilioretinal artery supplies the macula (10% of cases), central visual acuity may be preserved, but the visual field is severely constricted.
- BRAO: vision loss is sectoral, corresponding to the ischemic territory. Acuity may remain adequate if the macula is spared.
- Ophthalmic artery occlusion: the most severe presentation, with near-total vision loss, sometimes associated with ocular pain and ophthalmoplegia.
Episodes of amaurosis fugax (transient vision loss lasting a few minutes) may precede definitive retinal artery occlusion and should be considered a major warning sign requiring immediate ophthalmological consultation.
Diagnosis and examinations for retinal artery occlusion
Fundus examination
The diagnosis of retinal artery occlusion is primarily clinical. On fundus examination, the typical appearance of a CRAO shows a whitish retina due to ischemic edema, contrasting with a "cherry-red spot" at the macula — the fovea retaining its normal color thanks to the underlying choroidal vascularization. The retinal arteries may appear narrowed, thread-like, or even segmented. Intravascular emboli are visible in more than 50% of cases at arterial bifurcations.
OCT and OCT angiography
Optical coherence tomography (OCT) reveals hyperreflectivity of the inner retinal layers, indicating intracellular ischemic edema. Over time, it allows monitoring of progression toward retinal atrophy. OCT angiography (OCTA) provides a detailed, non-invasive analysis of retinal capillary perfusion, enabling precise mapping of non-perfusion zones in both the superficial and deep vascular networks. These imaging tools are particularly useful for assessing the severity of ischemia and monitoring disease progression.
Fluorescein angiography
Although not essential, fluorescein retinal angiography can demonstrate the extent of non-perfusion and circulatory delay. It is also useful for detecting multiple peri-arterial leakages suggestive of an inflammatory cause.
Systematic cardiovascular workup
The etiological workup is an essential component of the management of any retinal artery occlusion. It systematically includes: carotid duplex ultrasound, electrocardiogram, cardiac echocardiography, cerebral MRI with vascular sequences, and blood tests (blood glucose, lipid panel, inflammatory markers). In patients over 50 years of age, screening for giant cell arteritis (ESR, CRP) is imperative. In younger patients, a comprehensive thrombophilia workup is performed.
Treatment and management of retinal artery occlusion
Retinal artery occlusion is considered a stroke equivalent at the level of the eye. Its management must be immediate and multidisciplinary. It is important to emphasize that no treatment has, to date, formally proven its efficacy in restoring retinal circulation and recovering lost vision. Nevertheless, certain strategies are implemented:
- Intravenous thrombolysis: if the patient is seen within 4.5 hours of symptom onset, fibrinolysis may be considered in a neurovascular unit (injection of urokinase or rt-PA). A meta-analysis reports improvement in 50% of cases treated within this timeframe, compared to 17.7% without treatment.
- Emergency neurovascular management: cerebral MRI to screen for an associated stroke (present in 15 to 25% of cases), hospitalization if necessary.
- Emergency corticosteroid therapy: when giant cell arteritis is suspected, even before diagnostic confirmation.
- Etiological treatment: carotid surgery in cases of significant stenosis, anticoagulation, treatment of the underlying cardiac condition.
Former maneuvers (ocular massage, anterior chamber paracentesis, hyperbaric oxygen) are considered obsolete or even dangerous and should under no circumstances delay referral to a specialized unit. Control of cardiovascular risk factors (hypertension, diabetes, cholesterol, smoking) is fundamental for preventing recurrences and protecting the fellow eye.
Visual prognosis and long-term follow-up
The visual prognosis of retinal artery occlusion depends on the location and duration of ischemia. In CRAOs, visual acuity remains below 1/10 in 61% of cases. The presence of a functional cilioretinal artery improves the prognosis (47% improvement versus 16% without). Branch retinal artery occlusions have a significantly better prognosis: 80% of patients retain acuity greater than 5/10.
Beyond vision, the overall cardiovascular risk is significantly increased after retinal artery occlusion. The risk of coronary artery disease is doubled and that of carotid plaques is quadrupled. Regular cardiological follow-up is therefore essential. From an ophthalmological standpoint, neovascular glaucoma may develop in 2 to 5% of CRAO cases, usually within 6 weeks of the episode, justifying rigorous ophthalmological follow-up. As with other retinal vascular conditions such as diabetic retinopathy or retinal detachment, the speed of management determines the prognosis.
FAQ: Retinal artery occlusion
Is retinal artery occlusion an emergency?
Yes, retinal artery occlusion is an ophthalmological and vascular emergency. It is considered the equivalent of a stroke at the level of the eye. The retina can sustain irreversible damage within a few hours. If you experience sudden vision loss in one eye, seek emergency care immediately or call emergency medical services. Management within 4.5 hours may allow consideration of thrombolysis.
What are the first symptoms of retinal artery occlusion?
The main symptom is sudden, painless vision loss affecting one eye. Vision may be reduced to perceiving shadows or light. Episodes of transient vision loss (amaurosis fugax), lasting a few minutes before resolving spontaneously, may precede definitive occlusion and constitute a warning sign that should not be overlooked.
Can vision be recovered after retinal artery occlusion?
The visual prognosis depends on the type of retinal artery occlusion. In central artery occlusions without a cilioretinal artery, more than 60% of patients retain acuity below 1/10. In contrast, branch retinal artery occlusions have a better prognosis, with 80% of patients maintaining vision above 5/10. The presence of a functional cilioretinal artery and the speed of management favorably influence recovery.
What examinations are performed in cases of retinal artery occlusion?
The diagnosis is primarily based on fundus examination. OCT and OCT angiography allow analysis of the extent of retinal ischemia. A comprehensive cardiovascular workup is systematic: carotid duplex ultrasound, ECG, cardiac echocardiography, cerebral MRI, and blood tests. In patients over 50 years of age, screening for giant cell arteritis is imperative through ESR and CRP testing.
Is there an effective treatment for retinal artery occlusion?
To date, no treatment has formally proven its efficacy in restoring retinal circulation. Intravenous thrombolysis, considered within 4.5 hours of symptom onset, shows encouraging results with improvement in approximately 50% of cases. The major priority remains the etiological workup to prevent a stroke or involvement of the other eye, as well as control of cardiovascular risk factors.
What is the link between retinal artery occlusion and stroke?
Retinal artery occlusion shares the same mechanisms and risk factors as ischemic stroke. In 15 to 25% of cases, silent cerebral ischemic lesions are discovered during the imaging workup. The risk of coronary artery disease is doubled and that of carotid plaques is quadrupled. This is why any retinal artery occlusion requires a comprehensive cardiovascular workup and long-term cardiological follow-up.
How can retinal artery occlusion be prevented?
Prevention is primarily based on controlling cardiovascular risk factors: managing hypertension, diabetes, and cholesterol, quitting smoking, maintaining regular physical activity, and adhering to prescribed anticoagulant or antiplatelet treatments. Regular ophthalmological follow-up is also recommended, particularly in patients at vascular risk, in order to detect any asymptomatic retinal emboli.
When to consult Dr Julien Gozlan?
Any sudden vision loss, even transient (amaurosis fugax), constitutes an absolute emergency requiring immediate ophthalmological consultation. Dr Julien Gozlan recommends consulting without delay in cases of a sudden black curtain over one eye, sectoral vision loss, rapidly onset blurred vision, or after any episode of transient monocular blindness. These symptoms may reveal a retinal artery occlusion requiring an urgent workup. Specialized follow-up is also indicated for patients with significant cardiovascular risk factors, a history of stroke or transient ischemic attack, or retinal emboli discovered incidentally during a fundus examination.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan welcomes you at the Paris – Auteuil Ophthalmology Practice for the diagnosis, workup, and follow-up of retinal artery occlusions. Equipped with a state-of-the-art technical platform including the latest generation OCT and OCT angiography, he ensures rapid and coordinated management with neurovascular and cardiology teams to protect your vision and cardiovascular health.
Book an Appointment on DoctolibFurther reading
- OCT: optical coherence tomography: discover this key examination for analyzing retinal layers and monitoring the progression of retinal vascular diseases.
- OCT angiography: understand this non-invasive tool that maps retinal capillary perfusion without dye injection.
- Diabetic retinopathy: another common retinal vascular condition sharing risk factors with arterial occlusions.
- Retinal detachment: an ophthalmological emergency also requiring rapid management to preserve vision.