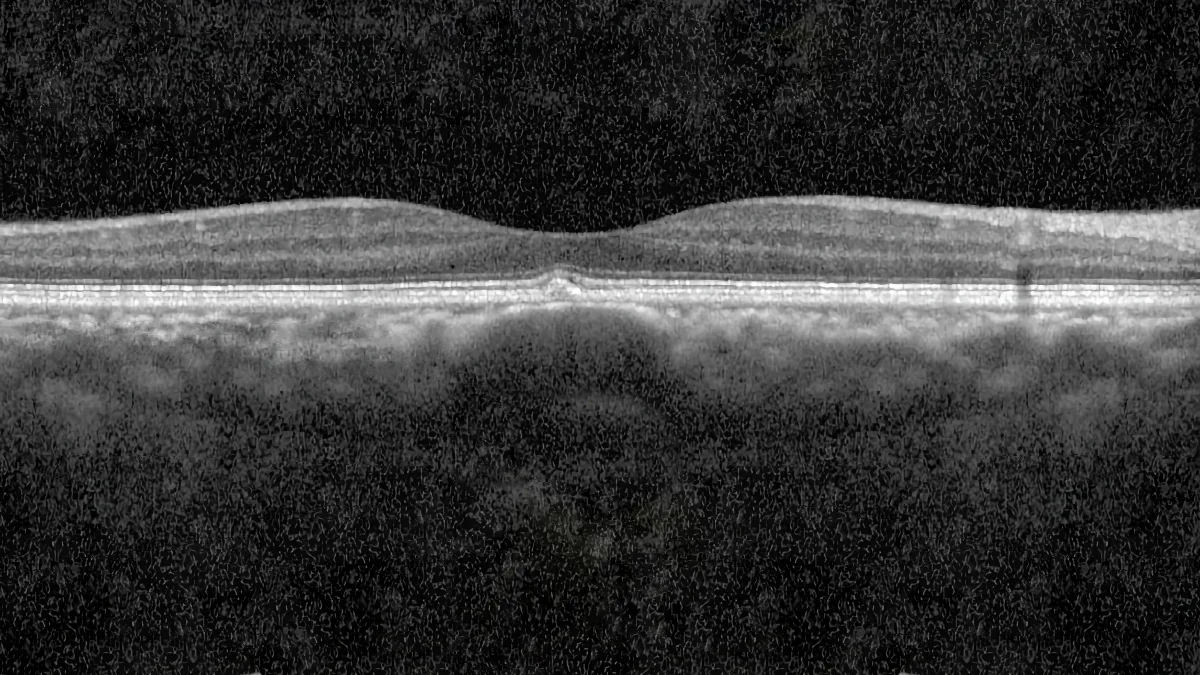
The pachychoroid spectrum encompasses a group of ocular conditions that share common abnormalities of the choroid, the vascular layer beneath the retina that provides nourishment. First described in 2013, this concept has profoundly changed our understanding of many retinal diseases. Julien Gozlan, M.D., an ophthalmologist specializing in retinal diseases at the Paris – Auteuil Ophthalmology Practice, offers in this article a clear and accessible explanation of what pachychoroid is, the different conditions that make up this spectrum, the examinations required for diagnosis, and the available treatments.
What is pachychoroid? Understanding the role of the choroid
To properly understand the concept of pachychoroid, one must first look at the choroid. It is a thin layer of vascular tissue located just behind the retina. Its role is essential: it supplies the oxygen and nutrients required for the proper functioning of photoreceptors, the cells that capture light and enable vision.
The choroid is composed of three layers of blood vessels, from the most superficial to the deepest:
- The choriocapillaris: a network of very small vessels in direct contact with the retina.
- Sattler's layer: medium-caliber vessels.
- Haller's layer: the large vessels, the choroidal veins.
The term "pachychoroid" comes from the Greek pachy, meaning "thick." It initially referred to an abnormal thickening of the choroid. Today, the definition is more precise: pachychoroid is characterized by the presence of dilated choroidal veins (called "pachyvessels") in Haller's layer, associated with compression of the choriocapillaris and dysfunction of the retinal pigment epithelium, the protective barrier between the choroid and the retina.
Conditions within the pachychoroid spectrum
The pachychoroid spectrum does not refer to a single disease, but rather a group of conditions that share these same choroidal abnormalities. There are uncomplicated forms and complicated forms, which can lead to significant vision loss.
Uncomplicated pachychoroid
In some cases, choroidal abnormalities are present without significant visual impact. These include:
- Pachychoroid epitheliopathy: subtle alterations of the pigment epithelium without fluid accumulation beneath the retina. Patients are generally asymptomatic.
- Pachydrusen: deposits beneath the pigment epithelium that are larger and more irregular than the classic drusen seen in AMD. They are characteristic of the pachychoroid spectrum and do not appear to increase the risk of neovascularization.
- Focal choroidal excavation: a localized thinning of the choroid, visible on OCT, usually without consequences for vision unless it involves the central zone.
Complicated pachychoroid
Complicated forms are those that cause decreased visual acuity and require management:
- Central serous chorioretinopathy (CSC): this is the most well-known condition within the spectrum. It primarily affects men between 30 and 50 years of age and presents with fluid accumulation beneath the retina. Stress, corticosteroid use, sleep disorders, and shift work are well-identified triggering factors. The acute form often resolves spontaneously within 3 to 6 months, but chronic forms can cause lasting vision impairment.
- Pachychoroid neovasculopathy: abnormal new vessels develop beneath the pigment epithelium. Unlike classic AMD, these neovessels occur in patients without typical drusen but with signs of pachychoroid. They present as an irregular elevation of the pigment epithelium visible on OCT.
- Polypoidal choroidal vasculopathy (PCV): formerly considered a form of AMD, it is now classified within the pachychoroid spectrum. It is characterized by aneurysmal dilations of the neovessels beneath the pigment epithelium, which can cause retinal hemorrhages.
- Peripapillary pachychoroid: a rarer form, described in 2018, characterized by retinal cysts and subretinal fluid localized around the optic nerve.
Diagnosis: how is pachychoroid detected?
Diagnosis is based on a comprehensive retinal imaging workup performed in the office. The key examinations are:
- OCT (optical coherence tomography): this is the fundamental examination. In EDI (enhanced depth imaging) mode or with Swept Source technology, it allows detailed visualization of the different choroidal layers, measurement of choroidal thickness, and identification of pachyvessels and choriocapillaris compression.
- OCT-angiography: this non-invasive examination allows visualization of retinal and choroidal vessels without dye injection. It is particularly effective for detecting pachychoroid neovascularization.
- Indocyanine green (ICG) angiography: it allows visualization of dilated choroidal veins in the early phases and areas of vascular hyperpermeability in the intermediate phases, which are characteristic of pachychoroid.
- Fundus autofluorescence: it highlights alterations of the pigment epithelium often associated with complicated forms.
It is the combination of these examinations that enables the retina specialist to establish a precise diagnosis and distinguish pachychoroid conditions from other causes of vision loss, particularly age-related macular degeneration.
Treatment of pachychoroid and its complications
Management varies depending on the diagnosed condition and its impact on vision.
Uncomplicated forms
Isolated epitheliopathy, pachydrusen, or choroidal excavation located outside the central zone generally do not require treatment. Regular monitoring with OCT is recommended, as these forms can progress to neovascular or exudative complications.
Central serous chorioretinopathy
The first step involves identifying and, where possible, eliminating triggering factors: discontinuation of corticosteroids (if medically feasible), stress management, and treatment of any sleep apnea syndrome. If subretinal fluid persists beyond 3 to 6 months with decreased visual acuity, the standard treatment is half-fluence photodynamic therapy (PDT), guided by ICG angiography.
Neovascularization and polypoidal choroidal vasculopathy
When neovascularization is present, treatment relies on intravitreal injections (IVT) of anti-VEGF agents, as in neovascular AMD. However, the treatment response may be less complete than in classic AMD. In resistant forms, a combined treatment associating intravitreal injections and photodynamic therapy may be offered to improve outcomes. Monitoring relies on regular OCT examinations to adjust the injection schedule.
Pachychoroid: a constantly evolving concept
It is important to emphasize that the pachychoroid spectrum is a relatively recent concept, and its definition continues to evolve. Current research suggests that there is a continuum between the different conditions within the spectrum: epitheliopathy may progress to CSC, which in turn may be complicated by neovascularization and then polypoidal choroidal vasculopathy. Genetic and hereditary factors also appear to play a role, and studies have identified susceptibility genes shared between pachychoroid and AMD.
Constant advances in retinal imaging, particularly wide-field imaging and OCT-angiography, allow increasingly detailed analysis of the choroid and should lead to a more objective definition of pachychoroid in the coming years. This improved understanding is already translating into more tailored therapeutic strategies for patients.
FAQ: Pachychoroid and the pachychoroid spectrum
What is pachychoroid in simple terms?
Pachychoroid refers to an abnormal state of the choroid, the vascular layer located beneath the retina. It is characterized by the dilation of large choroidal veins that compress the small nutrient vessels of the retina. This situation can lead to dysfunction of the pigment epithelium and, in some cases, visual complications.
Is pachychoroid a serious condition?
Not all forms of pachychoroid are serious. Uncomplicated forms (epitheliopathy, pachydrusen) are often asymptomatic and only require monitoring. However, complicated forms such as chronic central serous chorioretinopathy or neovascularization can impair vision and require appropriate treatment. Early diagnosis is essential to preserve visual function.
How is pachychoroid diagnosed?
Diagnosis relies primarily on OCT in EDI or Swept Source mode, which allows visualization of choroidal thickness and pachyvessels. OCT-angiography detects neovascularization without injection, and indocyanine green angiography reveals choroidal vascular hyperpermeability. These examinations are painless and performed directly in the office.
What is the difference between pachychoroid and AMD?
Although both conditions can be complicated by neovascularization, they have distinct mechanisms. AMD is related to aging of the macula with drusen accumulation, whereas pachychoroid is characterized by choroidal vascular abnormalities (dilated veins, compression of the choriocapillaris). Patients with pachychoroid generally have few or no drusen. This distinction is important because therapeutic management may differ.
Can pachychoroid be hereditary?
Recent studies have shown that pachychoroid may have a hereditary component. Susceptibility genes shared with AMD have been identified. However, research in this area is still ongoing and the precise genetic mechanisms remain to be elucidated.
What treatments are available for pachychoroid complications?
Treatment depends on the complication. For persistent central serous chorioretinopathy, half-fluence photodynamic therapy is the standard treatment. For neovascularization, intravitreal anti-VEGF injections are used, sometimes combined with photodynamic therapy in resistant forms. Elimination of triggering factors (corticosteroids, stress) is always recommended as a first-line measure.
How often should pachychoroid be monitored?
The monitoring schedule depends on the form of pachychoroid and its severity. Uncomplicated forms generally require a check-up every 6 to 12 months with OCT. Complicated forms, particularly neovascular ones, require closer follow-up, often monthly during the first months of treatment, in order to adjust injections and prevent any worsening.
When to consult Julien Gozlan, M.D.?
If you notice decreased vision, distortion of straight lines (metamorphopsia), a dark or blurry spot in the center of your vision, or if you have been informed of a choroidal abnormality during an eye examination, it is recommended to promptly consult a retina specialist. Early diagnosis of pachychoroid spectrum conditions allows for appropriate monitoring and, if necessary, treatment to preserve your visual function.
📍 Consultation at Paris – Auteuil Ophthalmology Practice
Julien Gozlan, M.D. sees patients at the Paris – Auteuil Ophthalmology Practice for the diagnosis and management of pachychoroid spectrum conditions. With a comprehensive technical platform including latest-generation OCT, OCT-angiography, and angiography, he provides thorough retinal assessments and personalized follow-up tailored to your situation.
Book an Appointment on DoctolibFurther reading
- AMD: understanding age-related macular degeneration: a condition often confused with pachychoroid complications.
- OCT: the gold standard examination in ophthalmology: discover how this examination allows detailed visualization of the choroid and retina.
- OCT-angiography: vascular imaging without injection: a key examination for detecting neovascularization within the pachychoroid spectrum.
- Intravitreal injections (IVT): procedure and indications: everything you need to know about this treatment used in neovascular forms.