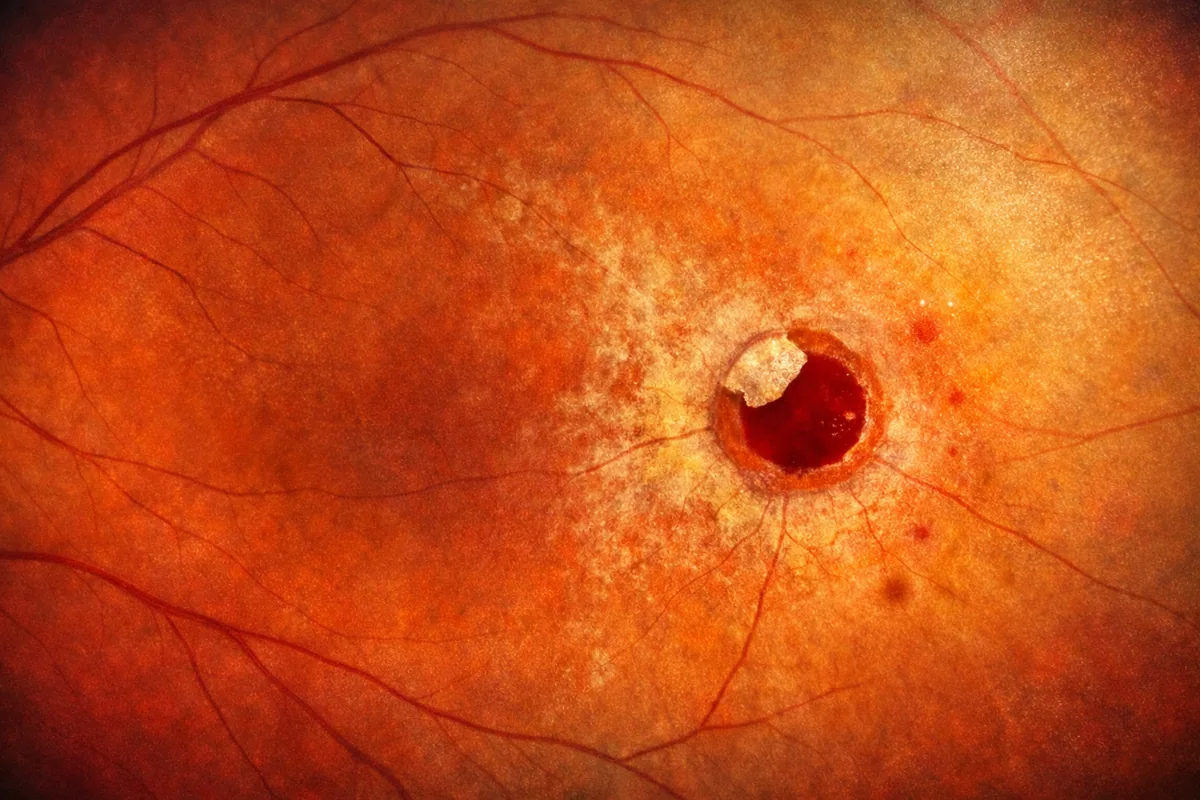
An operculated hole is a lesion of the peripheral retina caused by a posterior vitreous detachment (PVD). During this physiological process, the vitreous exerts traction on the retina and tears away a small fragment of retinal tissue, called an operculum, which remains suspended above the hole. This lesion is managed either through simple monitoring or preventive laser retinopexy performed in the office; surgery is only indicated in cases of associated retinal detachment. Julien Gozlan, M.D., ophthalmologist in Paris 16, explains in this article the mechanisms of formation, symptoms, diagnosis, and management of this peripheral retinal lesion.
What is an operculated hole?
An operculated hole corresponds to a full-thickness loss of substance in the peripheral retina. Its distinctive feature lies in its mechanism of formation: posterior vitreous detachment is directly responsible. When the vitreous gel separates from the retinal surface, it can exert sufficient focal traction to tear away a fragment of retina. This fragment, called the operculum, then floats in the vitreous cavity, directly above the hole.
This characteristic is fundamental because it clearly distinguishes an operculated hole from an atrophic retinal hole. The latter develops gradually through thinning and degeneration of retinal tissue, without active vitreous traction. It is frequently observed in the periphery of myopic patients' retinas, within areas of lattice degeneration. An atrophic hole does not have a floating operculum above it.
Mechanism of formation and risk factors
Posterior vitreous detachment occurs naturally with age, generally after 50–60 years. The vitreous, a transparent gel filling the ocular cavity, progressively liquefies and eventually separates from the retina. During this separation, areas of abnormally strong vitreoretinal adhesion may persist. The traction exerted on these anchor points can then tear away a piece of retina, creating an operculated hole.
The main risk factors include:
- Age: PVD becomes more common after age 50.
- Myopia: myopic eyes have vitreous that liquefies earlier.
- Previous ocular surgery: particularly after cataract surgery, PVD may occur sooner.
- Ocular trauma: an impact can accelerate the vitreous detachment process.
The sudden onset of floaters and photopsia (flashes of light) constitutes the typical clinical presentation of PVD and should alert the patient to the possibility of an associated tear or operculated hole.
Symptoms and diagnosis of an operculated hole
An operculated hole may be completely asymptomatic and discovered incidentally during a fundus examination. However, in most cases, the symptoms are those of the PVD that caused it:
- Sudden onset of floaters in the visual field.
- Flashes of light (photopsia) perceived in the periphery, especially in the dark.
- More rarely, a shadow or curtain in the peripheral visual field, which may suggest the onset of retinal detachment.
Diagnosis is based on a dilated fundus examination performed at the slit lamp with a contact lens or a three-mirror lens. The ophthalmologist identifies the round retinal hole in the periphery, topped by its floating operculum. OCT (optical coherence tomography) examination can complement the assessment by precisely visualizing the morphology of the hole and confirming the absence of residual vitreous traction on its edges.
Treatment and management
The management of an operculated hole is based on two main options, determined according to the size of the hole, its location, the presence or absence of subretinal fluid, and associated symptoms. It is essential to understand that this lesion does not require surgery in itself: only the occurrence of retinal detachment warrants surgical intervention.
Simple monitoring
In many cases, an operculated hole is considered a low-risk lesion for progression to retinal detachment. Indeed, since the operculum is detached and floating freely, there is no longer active vitreoretinal traction on the edges of the hole. The vitreous no longer pulls on the retina at that location. Julien Gozlan, M.D. may then recommend regular monitoring through fundus examination, without immediate treatment. The patient is informed of the warning signs (flashes of light, dark curtain, increase in floaters) that should prompt an emergency consultation.
Laser retinopexy (laser photocoagulation)
In certain situations — large hole, presence of perilesional subretinal fluid, high-risk location, or persistent symptoms — preventive laser retinopexy may be performed. This photocoagulation creates an adhesive scar around the operculated hole, preventing fluid from passing beneath the retina and thus preventing potential retinal detachment. Laser retinopexy is performed in the office, under topical anesthesia (eye drops), and takes a few minutes. It requires neither hospitalization nor prolonged time off from activities.
In cases of associated retinal detachment
If a retinal detachment has developed from the hole, the situation changes dramatically and urgent surgical management becomes necessary. A procedure such as vitrectomy or external surgery (scleral buckle) may then be indicated. However, this complication remains uncommon for isolated operculated holes, precisely due to the absence of residual vitreous traction.
Prognosis and outcome
The prognosis of an operculated hole is generally favorable. The absence of residual vitreous traction on the edges of the hole constitutes a major protective factor against retinal detachment. After laser retinopexy, the retinal scar consolidates within a few weeks and provides lasting protection. Regular ophthalmological follow-up remains essential, however, particularly in myopic patients or those with associated peripheral retinal lesions.
FAQ: Operculated hole
Is an operculated hole dangerous for vision?
An operculated hole is generally considered a low-risk lesion. The absence of active vitreous traction on its edges limits the risk of retinal detachment. However, regular ophthalmological monitoring is essential to detect any unfavorable progression. If there is any doubt, preventive laser retinopexy can be performed in the office.
What is the difference between an operculated hole and an atrophic hole?
An operculated hole results from vitreous traction during PVD, with tearing away of a retinal fragment (operculum) that floats above the hole. An atrophic hole, on the other hand, forms through progressive thinning of the retina, without traction, and typically occurs in the periphery in myopic patients. It does not have an operculum.
Is laser retinopexy painful?
Laser retinopexy is performed in the office after instillation of anesthetic eye drops. The procedure is generally well tolerated. Some patients may experience slight stinging or a sensation of discomfort. The procedure takes a few minutes and requires neither hospitalization nor prolonged time off from activities. Normal activities can be resumed quickly.
Can you drive after a diagnosis of operculated hole?
If your examination required pupil dilation, driving is not recommended for a few hours due to blurred vision and light sensitivity. Apart from this temporary effect, a stable operculated hole generally does not cause any driving limitations. Your ophthalmologist will provide you with personalized instructions.
Should you stop playing sports if you have an operculated hole?
In the absence of complications, moderate physical activity is generally permitted. However, sports with a risk of ocular trauma (combat sports, scuba diving) should be discussed with your ophthalmologist. After laser retinopexy, it is usually recommended to avoid intense exertion for a few days.
How often should an operculated hole be monitored?
The monitoring schedule is determined by your ophthalmologist based on the size of the hole, your degree of myopia, and the presence of other retinal lesions. Generally, a follow-up visit is scheduled a few weeks after the initial diagnosis, then every six months to one year. Any new symptoms (flashes, curtain, increase in floaters) should prompt an emergency consultation.
When to consult Julien Gozlan, M.D.?
Certain symptoms should prompt you to quickly consult a retina specialist ophthalmologist: sudden onset of floaters or a sharp increase in their number, perception of repeated flashes of light especially in peripheral vision, sensation of a dark curtain or veil progressing across the visual field, or a history of an operculated hole in the other eye or retinal detachment in the family.
📍 Consultation at Paris – Auteuil Ophthalmology Practice
Julien Gozlan, M.D. sees patients at Paris – Auteuil Ophthalmology Practice, 4 rue Donizetti, 75016 Paris, for the diagnosis and management of operculated holes. With a comprehensive technical platform including OCT and fundus examination, he offers tailored monitoring or preventive laser retinopexy according to your situation.
Book an Appointment on DoctolibFurther reading
- Retinal detachment: causes, warning symptoms, and emergency surgical management.
- Vitrectomy: everything you need to know about this retinal surgery, its indications, and how it is performed.
- Macular hole: understanding this central retinal condition and its treatment options.
- Floaters: origins, symptoms, and when to be concerned about floaters.