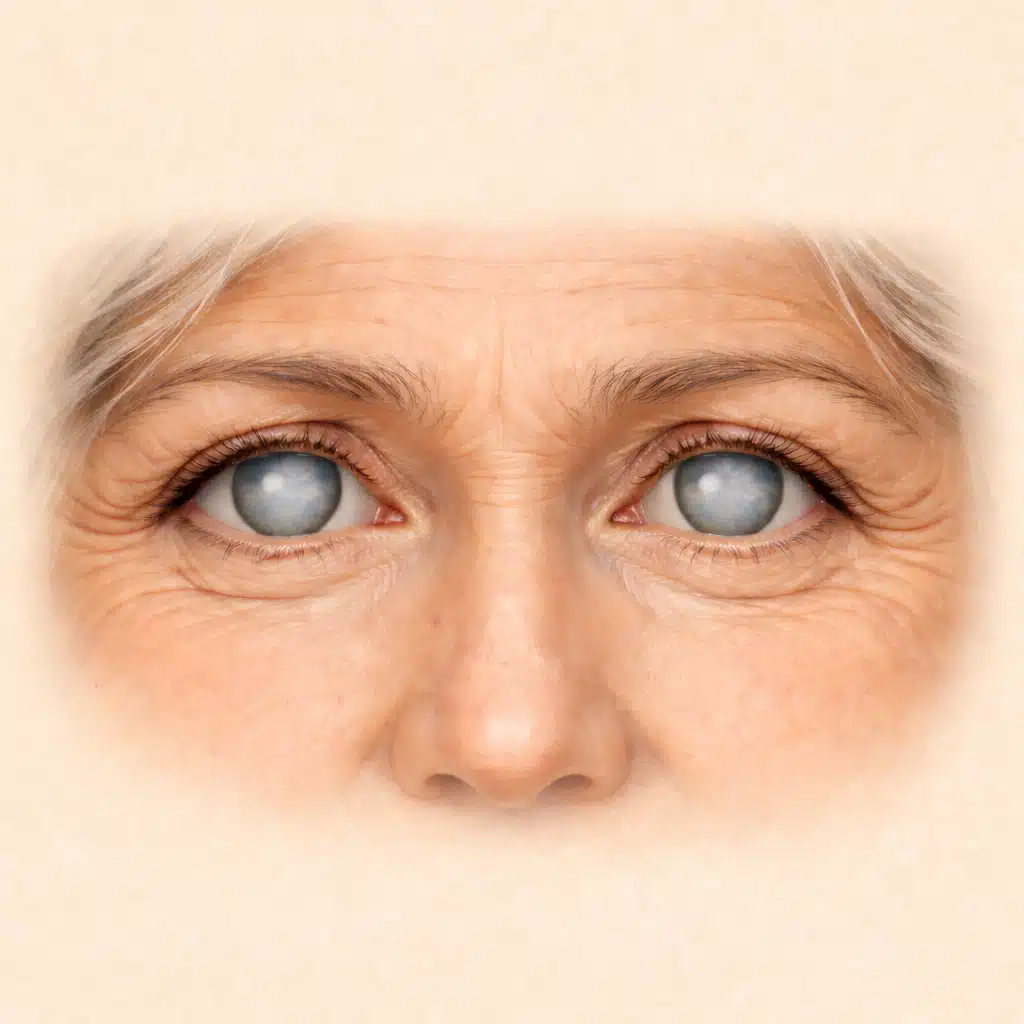
Cataract can affect one eye only (unilateral cataract) or both eyes (bilateral cataract), with different visual and practical consequences. Should one eye be operated on first, both eyes in succession, and at what pace? Julien Gozlan, M.D., ophthalmic surgeon in Paris 16, explains the specificities of unilateral and bilateral cataract, the reasonable intervals between the two procedures, and the situations where it is best not to wait too long for the second eye.
Unilateral vs. bilateral cataract: understanding the situation
A unilateral cataract refers to when only one eye presents significant opacification of the lens, while the other remains clear or minimally affected. Conversely, a bilateral cataract involves both lenses, sometimes asymmetrically (one eye more affected than the other).
In practice, this condition eventually becomes bilateral over the years, but it is common for one eye to "progress ahead." This asymmetry explains much of the discomfort experienced and guides the choice of timing and order of the procedures.
Symptoms: why unilateral cataract can be very bothersome
When cataract primarily affects only one eye, vision can become:
- blurry or hazy on one side only;
- with halos and glare, especially at night;
- sometimes with a significant change in prescription (the affected eye becoming more myopic, for example).
The brain tries to rely more on the clearer eye, but the asymmetry between the two eyes can cause:
- a sensation of double vision or overlapping images;
- significant visual fatigue, especially when using screens;
- discomfort when driving, particularly at night.
Thus, a unilateral cataract can sometimes be more poorly tolerated than a symmetrical bilateral cataract, because the difference between the two eyes disrupts binocular vision.
How to decide whether to operate on one or both eyes?
The decision does not rely solely on the number of affected eyes, but on the functional impact on daily life and on the examinations performed during the consultation.
Clinical and functional criteria
Julien Gozlan, M.D. takes several factors into account for unilateral or bilateral cataract:
- visual acuity of each eye (distance and near);
- perceived discomfort: reading, screen work, driving, sports;
- the difference in prescription between the two eyes (anisometropia);
- occupation and activities (night driving, precision work, high-level sports, etc.).
Generally, surgery is first proposed for the more affected eye (functionally unilateral cataract), then the other eye is scheduled at a later time, depending on residual discomfort.
Additional examinations and strategy
Beyond simple visual acuity measurement, the assessment relies on:
- precise ocular biometry for each eye, to determine lens implant power and refractive target (distance vision, mini-monovision, etc.);
- corneal topography in cases of astigmatism or prior refractive surgery;
- a macular OCT to check for any retinal pathology (AMD, macular edema, diabetic retinopathy, etc.);
- evaluation of the refractive target difference between the two eyes, to avoid excessive postoperative anisometropia.
These elements help define an overall visual plan: should the same correction be targeted for both eyes, or a slight difference to facilitate near vision? What is a reasonable interval between the two eyes to minimize discomfort?
Should both eyes be operated on the same day?
Simultaneous surgery on both eyes (same day) remains rare and is generally reserved for specific situations, depending on current guidelines, operating room organization, and the patient's profile.
In routine practice, sequential surgery is most often preferred:
- the more affected eye is operated on first;
- its recovery is assessed (visual acuity, comfort, intraocular pressure);
- then the second eye is scheduled shortly after if the bilateral cataract is bothersome.
This approach allows the strategy for the second eye (refractive target, implant choice) to be adjusted if needed based on the result of the first.
Bilateral cataract: ideal interval between the two eyes
In the case of bilateral cataract, the interval between the two procedures depends on:
- the level of discomfort in the second eye;
- the risk of anisometropia (difference in power between the two eyes after the first procedure);
- the patient's general health (diabetes, cardiovascular disease, ongoing treatments).
When a bilateral cataract is symmetrical and bothersome, it is often advisable not to space the two procedures too far apart, in order to:
- minimize discomfort between the two eyes;
- quickly regain stable binocular vision;
- then more precisely adjust any residual correction (glasses, progressive lenses).
Functionally unilateral cataract: when to propose surgery on the second eye?
It sometimes happens that only one eye is operated on while the other has only a moderate cataract. This is referred to as a functionally unilateral cataract after surgery.
The second eye is generally operated on when:
- the cataract in the second eye progresses and becomes bothersome;
- the difference between the two eyes becomes difficult to tolerate (impaired depth perception, fatigue);
- glasses correction is no longer sufficient to comfortably balance the two eyes.
The ideal timing is discussed during the consultation, based on the actual discomfort and the progression of the cataract in the second eye.
Visual prognosis: what can be expected?
In a bilateral cataract without any other ocular disease, the prognosis is generally excellent: once both eyes have been operated on, vision gains in brightness, contrast, and stability. Dependence on glasses can be reduced depending on the type of implant chosen.
In the presence of an associated condition (AMD, diabetic retinopathy, advanced glaucoma, etc.), cataract surgery can still provide improved comfort, but the final outcome will also depend on the condition of the retina and the optic nerve. This is one of the reasons why a comprehensive assessment before any decision is important.
Practical advice for patients
A few useful recommendations:
- report any significant functional discomfort (driving, work, reading) even if only one eye is affected;
- avoid excessively delaying surgery for a very bothersome bilateral cataract, as the impact on daily life can be considerable;
- after the first eye, clearly describe to the surgeon the comfort you experience (distance vision, near vision, imbalance between the eyes) to fine-tune the strategy for the second eye;
- strictly follow the postoperative treatment (eye drops, follow-up appointments) for each eye.
FAQ: unilateral vs. bilateral cataract
Is it always necessary to operate on both eyes in bilateral cataract?
Not necessarily right away. The most bothersome (or most advanced) eye is operated on first, then binocular visual comfort is reassessed. In practice, a progressive bilateral cataract often ultimately justifies surgery on both eyes, in order to restore stable overall vision (reading, driving, depth perception, visual fatigue).
Is it possible to never operate on the second eye?
Yes, if the cataract in the second eye remains minimal and not bothersome in daily life. However, cataract tends to progress over time: the question of a second procedure frequently arises later, especially if the difference between the two eyes becomes uncomfortable.
In unilateral cataract, is it dangerous to wait for the second eye?
In most cases, there is no life-threatening urgency for the eye. However, a highly asymmetric cataract can create significant functional discomfort (driving, sports, prolonged reading, visual fatigue), particularly due to an imbalance between the two eyes. If the discomfort becomes marked, it is generally advisable not to wait too long.
Why am I more bothered now that one eye has been operated on and the other has not?
Because the operated eye often sees more sharply and more brightly, while the other remains clouded by the cataract. This difference in brightness, contrast, and sometimes prescription (myopia/hyperopia/astigmatism) can cause a sensation of imbalance, visual fatigue, or difficulty with depth perception. This generally improves when the second eye is operated on (or after optical adjustment if the difference is small).
Can different refractive targets be chosen for each eye?
Yes, in some cases. The aim can be sharp distance vision in both eyes, or a mini-monovision approach (one eye made slightly more myopic to facilitate reading). The choice depends on your lifestyle, your tolerance for asymmetry, astigmatism, and the condition of the retina. This point must be discussed precisely before the procedure, as it influences day-to-day comfort.
How long should one wait between the two eyes?
It depends on the context (discomfort, professional activity, stability of the first eye, scheduling). In the case of a bothersome bilateral cataract, the second eye is often operated on within a few weeks to a few months, in order to quickly restore comfortable binocular vision and avoid an excessively long period of asymmetry.
Can I drive between the two procedures?
It depends on your overall visual acuity (with correction) and your comfort (glare, night vision, depth perception). A check-up can determine whether the driving criteria are met. If in doubt, it is wise to limit driving, particularly at night or on long trips, until stable binocular vision is achieved.
What should I do if I experience floaters, flashes of light, or a dark curtain after surgery?
These symptoms require an emergency consultation to rule out a retinal complication (tear, retinal detachment), especially in myopic patients or those with peripheral retinal degenerations. Do not wait for the scheduled appointment if the symptoms are recent, worsening, or accompanied by a decrease in vision.
When to consult Julien Gozlan, M.D.?
You can seek an opinion if you have a bothersome unilateral cataract, a bilateral cataract that has been mentioned to you, or if you are uncertain about the right time to operate on one or both eyes.
Julien Gozlan, M.D., ophthalmologist in Paris 16, performs a comprehensive assessment (visual acuity, biometry, topography, fundus examination, OCT if needed) and works with you to develop a personalized visual plan: order of procedures, interval between the two eyes, type of implant, and vision goals (distance, near, intermediate).
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Julien Gozlan, M.D. sees you at the Paris – Auteuil Ophthalmology Practice to assess your unilateral or bilateral cataract, discuss the ideal timing for operating on each eye, and choose with you the implant strategy best suited to your lifestyle.
Book an appointmentFurther reading
- Cataract: understanding everything about the condition before addressing the question of surgical strategy.
- Cataract surgery: procedure details, anesthesia, and postoperative course.
- Cataract implants: monofocal, toric, EDOF, and multifocal.
- Macular OCT: imaging examination to analyze the retina before surgery.