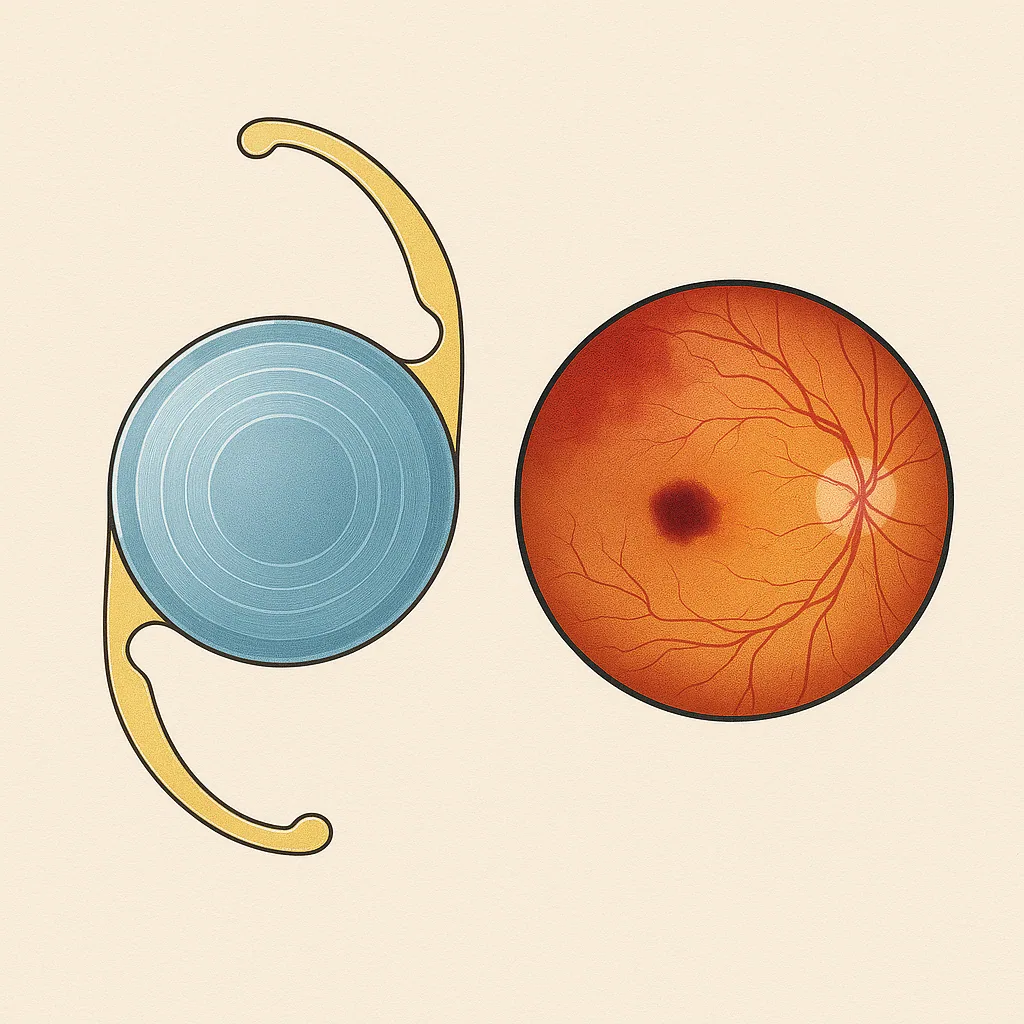
Age-related macular degeneration (AMD) and cataract are two very common eye diseases after age 60. Many patients ask the following question: AMD and cataract—is surgery risky? Could it worsen the macula? Dr Julien Gozlan, ophthalmic surgeon in Paris 16, summarizes what the scientific data show and what you need to know before undergoing surgery.
Overview: two different diseases
AMD affects the macula, the central area of the retina responsible for fine vision: reading, facial recognition, and driving. It can cause blurred central vision, distorted lines, or a dark spot in the center of the image.
Cataract refers to the progressive opacification of the crystalline lens, the eye's natural lens. Light is transmitted less effectively, and vision becomes hazy, dull, and sometimes yellowish. Surgery involves removing the cloudy lens and replacing it with a transparent intraocular lens implant.
AMD and cataract: does surgery worsen the disease?
For a long time, it was suspected that cataract surgery could accelerate the progression of macular disease. Modern studies involving large groups of patients followed over several years have not found a clear increase in the risk of progression to an advanced form in patients who underwent surgery compared to those who did not, when age and risk factors are comparable.
In practice, when a bothersome cataract coexists with stable AMD, surgery is often beneficial: vision becomes brighter, contrast improves, and daily activities become more comfortable. The macula must continue to be monitored, but cataract surgery is not considered a direct cause of worsening.
Why does it sometimes seem like the condition worsens after surgery?
After surgery, the image reaching the retina is clearer. Macular lesions that were "hidden" by the cataract become visible on examination and more noticeable to the patient. It may then seem as though AMD has suddenly progressed, when in fact it was already present.
Additionally, improved visual acuity can sometimes make distortions (metamorphopsia) or the central spot more apparent. This perception does not necessarily indicate acceleration of the disease, but rather a sharper awareness of the symptoms.
Macular OCT: the essential examination before surgery
Before cataract surgery in a patient with AMD (or suspected macular disease), the most useful examination is macular OCT. It allows in-depth analysis of the macula, even when the cataract impairs the quality of the fundus examination.
OCT can reveal:
- drusen (small deposits) consistent with an early form;
- signs of atrophy (advanced dry form);
- pigment epithelial detachment;
- intraretinal or subretinal fluid, suggestive of an exudative form;
- scarring changes that explain a limited visual prognosis.
This examination helps distinguish what is caused by the lens (cataract) from what is truly related to the macula (AMD).
What cataract surgery can improve… and what it cannot
Cataract surgery primarily improves:
- the sensation of haze and fog;
- brightness of vision;
- contrast;
- glare caused by lens opacity.
However, it does not "repair" macular lesions. If AMD is advanced, central vision may remain limited despite technically flawless surgery. The goal is then primarily to improve visual comfort and quality of life.
Yellow-tinted implants (blue light filters): useful for AMD?
Some intraocular lens implants are tinted yellow and filter part of the blue light. They have been proposed to protect the retina and slow, over the long term, the progression of macular degeneration.
Available data do not show, to date, a clear benefit of these filters in preventing or slowing the progression of AMD. However, these implants do not appear to be harmful to visual quality and may slightly reduce glare in some patients.
Exudative AMD and injections: can surgery still be performed?
In patients with exudative AMD treated with intravitreal injections, cataract surgery remains possible. It simply needs to be planned at the right time.
In practice, surgery is preferably performed when the disease is stabilized: no significant fluid on OCT, well-calibrated treatment, and regular follow-up. Once the cataract is removed, monitoring of the macula is often more reliable.
Management if you have both AMD and cataract
Before any surgical decision, a comprehensive assessment is performed: fundus examination, macular OCT, visual acuity measurement, and analysis of the functional impact of the cataract. Surgery is recommended when the haze caused by the cloudy lens interferes with daily life: reading, getting around, and sometimes driving.
After surgery, AMD is monitored as before, with regular check-ups, possible injections in case of an exudative form, and self-monitoring at home using an Amsler grid. Cataract surgery does not prevent continuing treatments or detecting disease progression.
FAQ: frequently asked questions about AMD and cataract
In which cases is cataract surgery truly beneficial when you have AMD?
The indication does not depend solely on the stage of AMD, but on how you use your eyes on a daily basis. Surgery is primarily considered when the cataract concretely limits your activities: reading, cooking, getting around outdoors, occasional driving, manual tasks, etc. Even if AMD limits maximum visual acuity, gaining brightness and visual comfort can make a real difference in everyday life. Conversely, if the cataract causes little inconvenience in daily life, it may be reasonable to postpone surgery and focus on macular monitoring and any AMD treatments.
How is the visual goal determined when you have both cataract and AMD?
The goal is not the same as for a patient without AMD. Rather than aiming for "20/20 without glasses," the objective is to achieve the best possible functional vision given the condition of the macula. In practical terms, specific situations are discussed: reading a few lines with good lighting, recognizing a face at a reasonable distance, moving objects in the kitchen, seeing steps or curbs. The macular assessment helps anticipate whether the expected improvement will be modest or more significant, and to adjust expectations to avoid false promises while still benefiting from cataract surgery when appropriate.
Does management change if my AMD is already being treated with intravitreal injections?
Yes, the approach is somewhat adapted, without ruling out the possibility of surgery. When you are receiving intravitreal injections for an exudative form of AMD, surgery is generally planned during a phase of stability: macular fluid well controlled on OCT, regular injection schedule, no recent flare-up. Injection sessions are then rescheduled around the surgery date to avoid interrupting treatment longer than necessary. In practice, cataract and AMD are therefore managed together, with a coordinated schedule between surgery, OCT check-ups, and injections.
What type of implant is preferred when you have AMD?
In the presence of AMD, the primary goal is to achieve the sharpest and most contrasted image possible on the compromised macula. This is why monofocal implants are almost always preferred, possibly with a slight trade-off to facilitate a particular distance (for example reading or computer screen use), rather than multifocal implants. The choice of a possible yellow filter or a slightly different correction between the two eyes is discussed on a case-by-case basis depending on your habits (reading, screens, night driving) and the condition of each eye. The goal remains to find the most comfortable optical profile for your AMD, without altering the disease itself.
Are there any special recovery precautions when you have AMD?
Recovery after cataract surgery is generally the same as for a patient without AMD (eye drops, ocular hygiene, avoiding trauma, etc.), but macular monitoring is more frequent. After the immediate postoperative phase, more frequent OCT scans may be recommended to verify that the macula does not show any new leakage or worsening of AMD. At home, it is helpful to continue monitoring each eye separately, for example with an Amsler grid, and to promptly report any unusual visual changes (more pronounced distortions, central spot, sudden decrease in vision). The idea is to benefit from the improved lens clarity while remaining highly responsive in case of macular changes.
Do I need to adjust my glasses or visual aids after surgery?
Yes, an optical reassessment is almost always necessary. Once the cataract is removed, the correction you need is no longer the same, and AMD may make low vision aids useful: magnifiers, tinted filters, enhanced lighting, video magnifiers, etc. These adjustments are discussed after postoperative stabilization, once vision has settled. In some patients, the combination of well-performed cataract surgery and well-chosen optical aids can restore more comfortable reading or greater independence in daily tasks, even if AMD limits purely measured central vision.
When to consult Dr Julien Gozlan
You may seek a specialist opinion if a cataract has been diagnosed and you already have macular involvement, or if you have been told about AMD without knowing whether surgery is advisable. Symptoms such as hazy vision, a foggy sensation, as well as wavy lines or a spot in the center of your visual field should prompt a consultation.
Dr Julien Gozlan, ophthalmologist in Paris 16, performs a comprehensive examination of your eyes, evaluates the respective importance of the cataract and macular disease, and provides you with personalized guidance on the benefit and optimal timing of potential surgery.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan sees you at the Paris – Auteuil Ophthalmology Practice to assess your cataract, possible AMD, and the most suitable intraocular lens implant for your situation.
Book an AppointmentFurther reading
- Age-related macular degeneration (AMD): symptoms, diagnosis, and management.
- Cataract surgery: procedure, implants, and recovery.
- Macular OCT: the key examination for analyzing the central retina.
- Association DMLA: additional information and resources for patients.