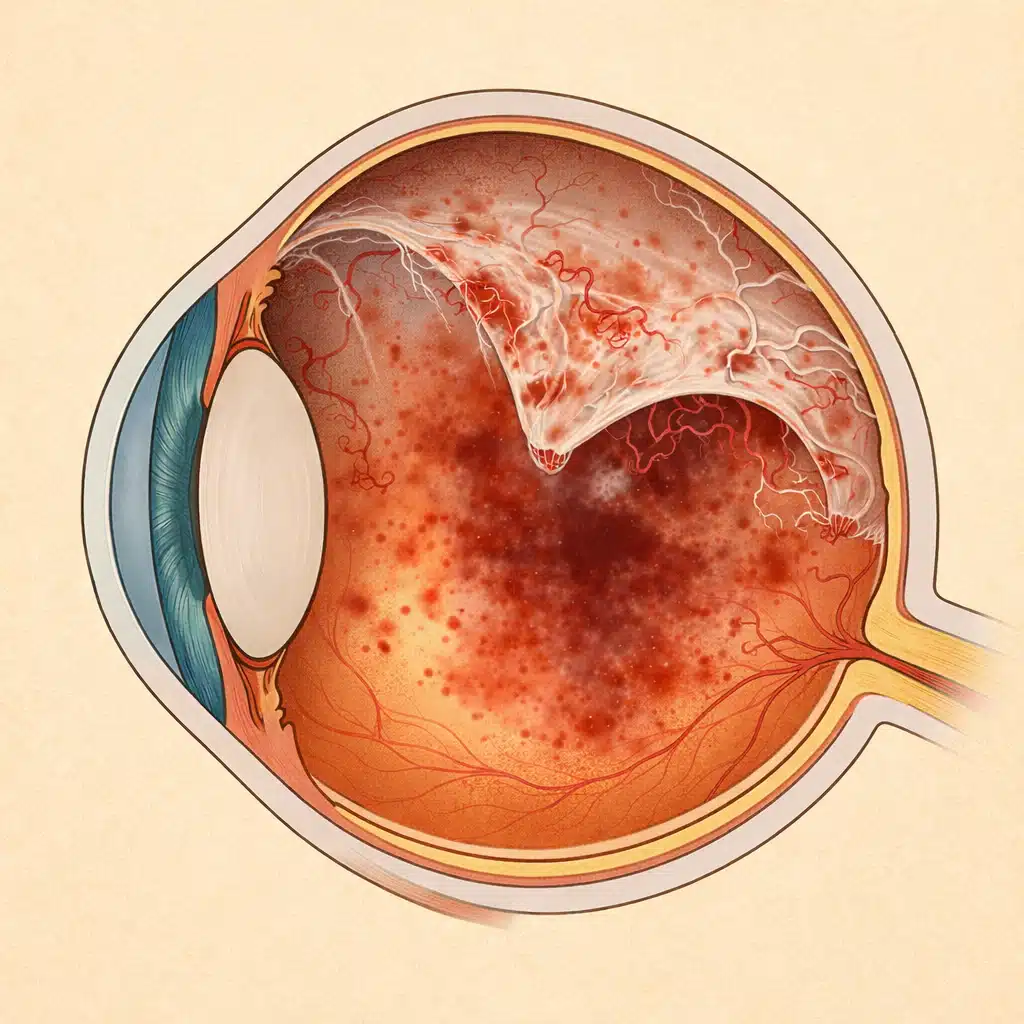
Diabetic retinopathy is a common and potentially severe complication of diabetes. When intravitreal hemorrhages recur or vascular proliferation becomes significant, a vitrectomy may be necessary to save or stabilize vision. Julien Gozlan, M.D., ophthalmic surgeon in Paris 16, explains the role of vitrectomy in diabetic retinopathy, its indications, procedure, and visual prognosis.
Diabetic retinopathy: a brief overview
Diabetic retinopathy refers to the progressive damage to the retinal blood vessels caused by diabetes. It is classically divided into:
- non-proliferative diabetic retinopathy: microaneurysms, punctate hemorrhages, exudates;
- proliferative diabetic retinopathy: development of abnormal neovascularization on the surface of the retina or the optic disc;
- diabetic macular edema, responsible for decreased central vision.
Neovessels are fragile, bleed easily into the vitreous, and may be associated with tractional membranes on the retinal surface, potentially leading to tractional detachment.
What is a vitrectomy?
A vitrectomy is a posterior segment surgery that involves removing the vitreous (the transparent gel) and directly treating the retina. It is most commonly performed under regional anesthesia (the eye is numbed while the patient remains awake).
Through very small incisions (micro-incisions), the surgeon introduces:
- a vitrectomy probe (to cut and aspirate the vitreous);
- a light pipe (to illuminate the vitreous cavity);
- potentially other instruments (forceps, scissors, laser probes).
At the end of the procedure, the eye is filled with clear fluid, or sometimes with a temporary gas or silicone oil depending on the case.
When does diabetic retinopathy require a vitrectomy?
Vitrectomy is not systematic in diabetic retinopathy. It is considered in certain advanced situations, for example:
- dense vitreous hemorrhage that does not resolve and prevents visualization of the retina;
- recurrent hemorrhages despite appropriate treatment;
- tractional retinal detachment involving or threatening the macula;
- significant vitreoretinal traction with risk of retinal tear;
- association with resistant diabetic macular edema, when traction plays a major role.
In practice, vitrectomy is discussed when vision is severely compromised or threatened and when conventional treatments (photocoagulation, intravitreal injections) are no longer sufficient.
OCT findings and surgical decision-making
Macular OCT and associated imaging play a central role in the decision to operate. The following findings are particularly important:
- diabetic vitreomacular traction: distortion of the inner layers, shearing;
- epiretinal membranes associated with folds or localized tractional detachment;
- partial or complete tractional macular detachment;
- macular edema with an obvious tractional component;
- assessment of outer layer integrity (external limiting membrane, ellipsoid zone) to evaluate visual prognosis.
The decision to proceed with vitrectomy takes into account:
- clinical findings (visual acuity, functional impact);
- OCT imaging and possible fluorescein angiography;
- diabetes control and the overall medical context;
- response to appropriate medical treatment (laser, intravitreal injections).
How is a vitrectomy for diabetic retinopathy performed?
The procedure is performed in a specialized surgical setting. The main steps are:
1) Placement of micro-incisions
Three small incisions are made in the sclera (white of the eye) to introduce the instruments. They are fine enough to often be self-sealing.
2) Removal of the vitreous and hemorrhages
The vitreous is progressively removed, particularly the areas opacified by blood. This helps clear the visual axis and visualize the underlying retina.
3) Treatment of membranes and traction
Tractional membranes on the retinal surface are carefully grasped and cut. The goal is to release the traction that is distorting or detaching the retina.
4) Endolaser photocoagulation
Endolaser treatment is often performed during the vitrectomy to complete or reinforce panretinal photocoagulation. This helps reduce neovascular activity and limit the risk of recurrence.
5) Final tamponade of the eye
At the end of the procedure, the eye is filled with saline solution, gas, or more rarely silicone oil depending on retinal stability and the type of detachment treated.
Postoperative course and recovery
After vitrectomy, treatment with antibiotic and anti-inflammatory eye drops is prescribed. Redness, a foreign body sensation, or blurred vision are common in the first few days.
If an intraocular gas tamponade is used, a bubble will be visible in the visual field and vision will remain partially blurred until it resorbs. Certain positioning may be recommended depending on the location of the treated lesions.
Vision then gradually improves over several weeks, sometimes several months, depending on the initial condition of the retina and the macula.
Visual prognosis: what can reasonably be expected?
The prognosis depends on several factors:
- duration and severity of diabetic retinopathy;
- presence of tractional macular detachment and its duration;
- integrity of the outer retinal layers on OCT;
- diabetes control and cardiovascular risk factors;
- possible associated conditions (glaucoma, AMD, etc.).
In many cases, vitrectomy at a minimum helps to stabilize the situation and prevent major deterioration. When the macular structures are still preserved, a significant improvement in vision is possible, but rarely to the point of "perfect" vision.
Frequently asked questions: vitrectomy and diabetic retinopathy
Is this an emergency surgery?
It depends on the situation. Prompt management is necessary in cases of tractional detachment threatening the macula, tractional macular detachment, massive vitreous hemorrhage with sudden vision loss, or if a severe underlying condition is suspected (combined tractional-rhegmatogenous detachment, significant traction, etc.). Other situations can be scheduled after optimizing diabetes control, cardiovascular treatment, and overall health.
Does vitrectomy cure diabetic retinopathy?
No. Vitrectomy primarily treats the complications of diabetic retinopathy (hemorrhages, fibrovascular membranes, traction, detachment), but the underlying disease persists. Controlling diabetes (blood glucose, HbA1c), blood pressure, and cardiovascular risk factors remains essential to limit recurrence and protect the fellow eye.
Is there a risk of new hemorrhage after surgery?
Yes, recurrent hemorrhages can occur, especially if neovascular activity remains significant or if retinal laser treatment is incomplete. Thorough panretinal photocoagulation, sometimes combined with intravitreal injections depending on the context, and good diabetes control reduce this risk. Postoperative follow-up is specifically designed to detect recurrence promptly.
Will I be able to return to work quickly?
It depends on your activity (screen work, driving, precision work, heavy lifting), which eye was operated on, and whether or not a tamponade (air/gas/oil) was used. A recovery period of a few days to a few weeks is common and may be longer if vision takes time to recover (dense hemorrhage, macular involvement, intraocular gas, complex surgery). Return to work is decided on a case-by-case basis, depending on visual recovery and professional requirements.
Is vitrectomy painful?
The procedure is performed under local anesthesia (most often) or sometimes general anesthesia, so it is not painful during surgery. The postoperative period may involve discomfort, a feeling of eye "fatigue," grittiness, or irritation, generally well controlled with eye drops and simple pain relievers. However, significant or increasing pain should prompt an immediate follow-up consultation.
Does diabetes need to be well controlled before surgery?
Yes, as much as possible. Good glycemic control (and blood pressure control) reduces the risk of complications, promotes healing, and improves retinal stability. In emergency situations, a "perfect" balance is not always achievable, but every effort is made to quickly optimize the patient's overall condition in coordination with the primary care physician or diabetologist.
Does vitrectomy prevent intravitreal injections afterward?
No. It is entirely possible to continue intravitreal injections if needed, for example in cases of persistent or recurrent diabetic macular edema, or to control neovascular activity. Vitrectomy and injections are complementary treatments, used as needed throughout the follow-up period.
Can cataract surgery be performed at the same time as vitrectomy?
In some cases, yes. Combined cataract and vitrectomy surgery may be offered when the cataract impedes access to the retina, when it is already significant, or when rapid cataract progression is anticipated after vitrectomy (especially in older patients). The decision depends on age, lens clarity, retinal complexity, and visual goals.
When should you consult Julien Gozlan, M.D.?
You should seek a specialized evaluation if:
- your ophthalmologist has mentioned proliferative diabetic retinopathy;
- you have experienced a vitreous hemorrhage with sudden vision loss;
- you have been told about retinal traction or tractional detachment;
- despite laser treatment and injections, your vision remains very reduced or continues to deteriorate.
Julien Gozlan, M.D., at the Paris – Auteuil Ophthalmology Practice, performs a comprehensive retinal assessment (fundus examination, OCT, complementary imaging) and discusses with you the potential benefit of vitrectomy and its objectives.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Julien Gozlan, M.D. sees you at the Paris – Auteuil Ophthalmology Practice to evaluate your diabetic retinopathy, interpret your examinations (OCT, angiography), and discuss potential surgical treatment by vitrectomy.
Book an AppointmentFurther reading
- Diabetic retinopathy: mechanisms, symptoms, and screening.
- Diabetic macular edema: the role of intravitreal injections.
- Intravitreal injections: procedure, efficacy, and follow-up.
- Vitrectomy: general principles of vitreous and retinal surgery.