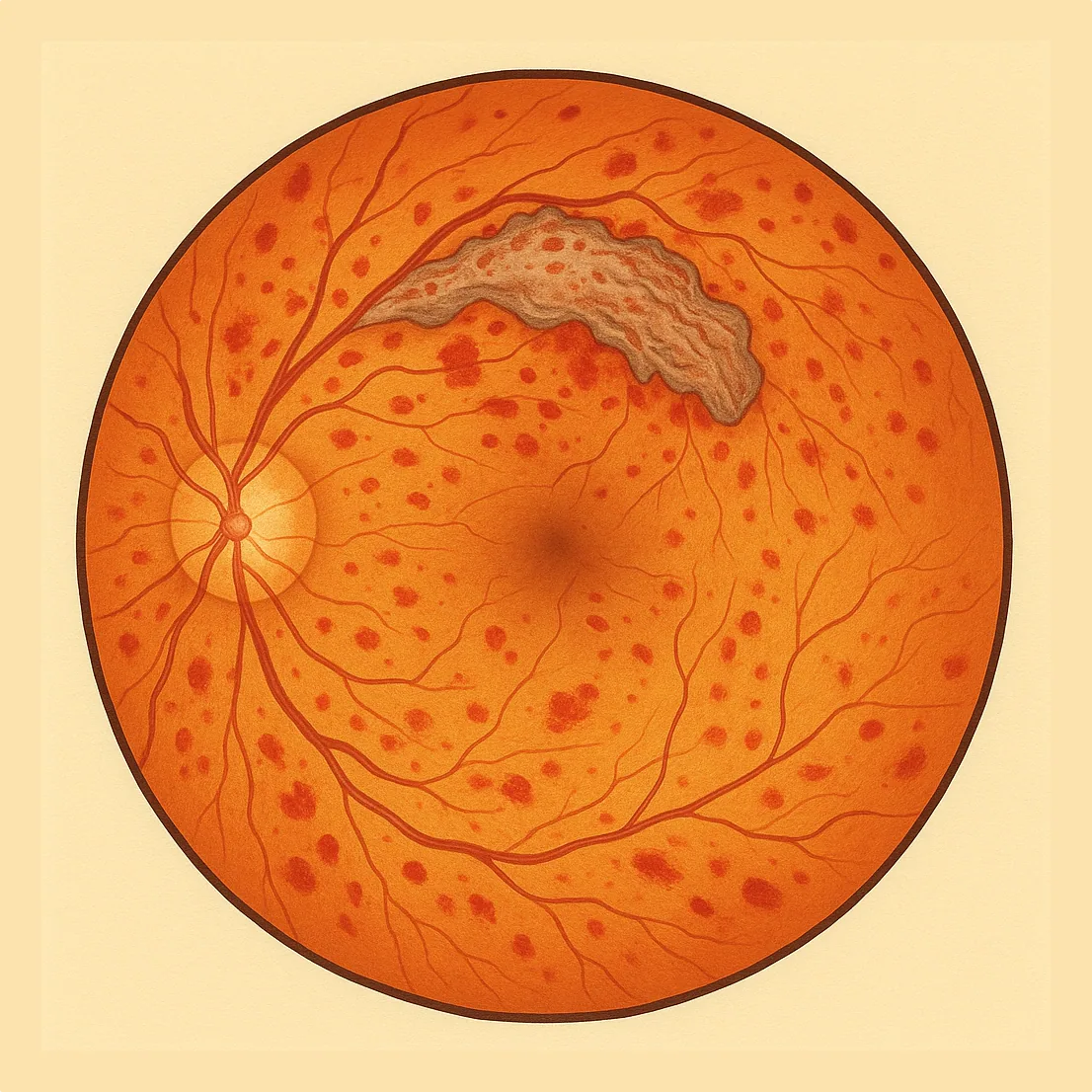
Diabetic retinopathy is a complication of diabetes that affects the small blood vessels of the retina. Often silent in its early stages, it can threaten vision if not detected and treated in time. Julien Gozlan, M.D., ophthalmologist at the Paris – Auteuil Ophthalmology Practice, provides a clear explanation of the stages, symptoms, screening, and available treatments.
What is diabetic retinopathy?
Diabetic retinopathy refers to progressive damage to the retinal capillaries caused by long-term hyperglycemia. It is classically divided into a non-proliferative form (early stages) and a proliferative form (advanced stage with neovascularization). Macular edema can occur at any point during the disease's progression and may cause a decrease in central vision.
Risk factors and the importance of screening
The risk increases with the duration of diabetes, poor glycemic control (elevated HbA1c), high blood pressure, hypercholesterolemia, and smoking. Pregnancy in a diabetic patient requires close monitoring. Regular screening helps identify diabetic retinopathy before symptoms appear and prevents complications.
Signs and symptoms of diabetic retinopathy
In the early stages, there are often no symptoms. On examination, microaneurysms (small red dots), hemorrhages, exudates, cotton-wool spots, venous abnormalities, and intraretinal microvascular abnormalities (IRMA) may be observed. When the macula is affected (edema), decreased vision, distortion of straight lines, and sometimes a central dark spot may appear. At the proliferative stage, new blood vessels can bleed (vitreous hemorrhage) or exert traction on the retina.
How is diabetic retinopathy diagnosed?
Diagnosis is based on a fundus examination and retinal photography. Macular OCT (retinal scan) measures any edema and monitors its progression. Depending on the case, fluorescein angiography (with dye) or OCT-A (dye-free angiography) may be used to determine the extent of ischemia and the presence of neovascularization. These examinations guide the treatment of diabetic retinopathy.
Treatments for diabetic retinopathy
1) Intravitreal injections
Anti-VEGF agents and, in some cases, corticosteroids administered as intravitreal injections reduce macular edema and stabilize vision. The treatment protocol is tailored to each patient (loading phase followed by a personalized schedule).
2) Retinal laser (photocoagulation)
Panretinal argon laser photocoagulation treats the proliferative form by reducing the ischemia responsible for neovascularization. Focal or grid laser may be used around the macula for certain vascular leaks. Laser treatment reduces the risk of hemorrhage, tractional retinal detachment, and neovascular glaucoma.
3) Vitrectomy
In cases of persistent vitreous hemorrhage or tractional retinal detachment threatening the macula, a surgical procedure called vitrectomy may be necessary to restore anatomical conditions favorable to vision.
Follow-up and daily prevention
Overall systemic control is essential: aim for an HbA1c close to the target set with your diabetologist, normalize blood pressure and lipid levels, and stop smoking. Regular ophthalmological follow-up is recommended: at least annually in the absence of retinal involvement, and more frequently if diabetic retinopathy is present or during pregnancy. Do not wait for symptoms to appear before seeking a consultation.
FAQ: frequently asked questions about diabetic retinopathy
How often should I have an eye examination if I have diabetes?
The frequency depends on your type of diabetes, how long you have had it, and whether diabetic retinopathy is already present. In the absence of retinal involvement, an examination at least once a year is generally recommended. If retinopathy is already present, or in the case of pregnancy in a diabetic patient, the schedule may be shortened to every 3 to 6 months. Your ophthalmologist will determine the appropriate frequency based on fundus photographs, OCT findings, and your glycemic control (HbA1c).
Can diabetic retinopathy develop even if my diabetes is well controlled?
Yes, well-controlled diabetes significantly reduces the risk of diabetic retinopathy but does not eliminate it entirely, especially when the disease has been present for a long time. Past hyperglycemia may have already weakened the retinal capillaries. This is why screening remains essential, even with good HbA1c levels, in order to detect early lesions that have not yet caused visual symptoms and to intervene at the right time if necessary.
Is diabetic retinopathy painful?
No, diabetic retinopathy is generally painless. This is in fact one of its pitfalls: the eye does not hurt, it is not red, and vision can remain good for a long time even though the retinal blood vessels are already being damaged. Pain only occurs in certain advanced complications (for example, neovascular glaucoma), which underscores the importance of not waiting for pain or significant vision loss before seeking regular examinations.
Can I drive if I have diabetic retinopathy?
Driving depends primarily on your visual acuity and visual field, not solely on the diagnosis of diabetic retinopathy. Many patients can continue to drive normally, sometimes with appropriate corrective lenses, as long as the legal vision requirements are met. However, in cases of significant macular edema, vitreous hemorrhage, or marked vision loss, driving may become dangerous. Your ophthalmologist can provide specific guidance and, if needed, recommend a temporary or permanent driving restriction depending on the situation.
What should I change in my daily life if I have been diagnosed with diabetic retinopathy?
A diagnosis of diabetic retinopathy is a signal to strengthen everything that protects your eyes in the long term. This includes: better glycemic control (in coordination with your diabetologist), managing blood pressure and cholesterol, quitting smoking, engaging in appropriate physical activity, and maintaining a balanced diet. Regarding vision, it may be helpful to optimize your eyeglass prescription, improve lighting (for reading, cooking, and working), and adapt certain daily tasks if vision loss is present. These measures complement any ocular treatments (laser, intravitreal injections, vitrectomy).
Are intravitreal injection or laser treatments compatible with my other medications?
In most cases, yes. Intravitreal injections and retinal laser treatment are usually compatible with other systemic treatments (insulin, oral antidiabetic medications, antihypertensives, anticoagulants). You should never stop a cardiac or anticoagulant medication on your own without medical advice. Always inform your ophthalmologist of your complete medication list and medical history (cardiac, vascular, surgical) so that appropriate precautions can be taken, in coordination with your general practitioner or diabetologist if needed.
Can diabetic retinopathy be completely cured?
The lesions associated with diabetic retinopathy are often chronic: the goal is stabilization rather than complete cure. However, with proper treatment (diabetes control, intravitreal injections, laser, and possibly vitrectomy), it is possible in many cases to preserve vision over the long term and prevent severe forms (vitreous hemorrhage, tractional retinal detachment, neovascular glaucoma). The objective is therefore to slow or halt disease progression rather than to completely eliminate all traces of the condition, which is why regular follow-up remains important even when vision is considered stable.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Julien Gozlan, M.D. performs screening, follow-up, and treatment of diabetic retinopathy (OCT, laser, injections) with a personalized protocol to preserve your vision.
Book an AppointmentFurther reading
- Diabetic macular edema: a common cause of vision loss in diabetic retinopathy.
- Intravitreal injections: anti-VEGF agents and corticosteroids.
- Macular OCT: the key examination for diagnosing and monitoring macular edema.