Angioid streaks are a rare but potentially serious ocular condition caused by breaks in Bruch's membrane at the back of the eye. Dr Julien Gozlan, ophthalmic surgeon specializing in retinal diseases in Paris 16, regularly sees patients affected by this condition. In this article, we explain in simple terms what angioid streaks are, their causes, the symptoms that should raise concern, the examinations required for diagnosis, and the treatments available today to preserve your vision.
What are angioid streaks?
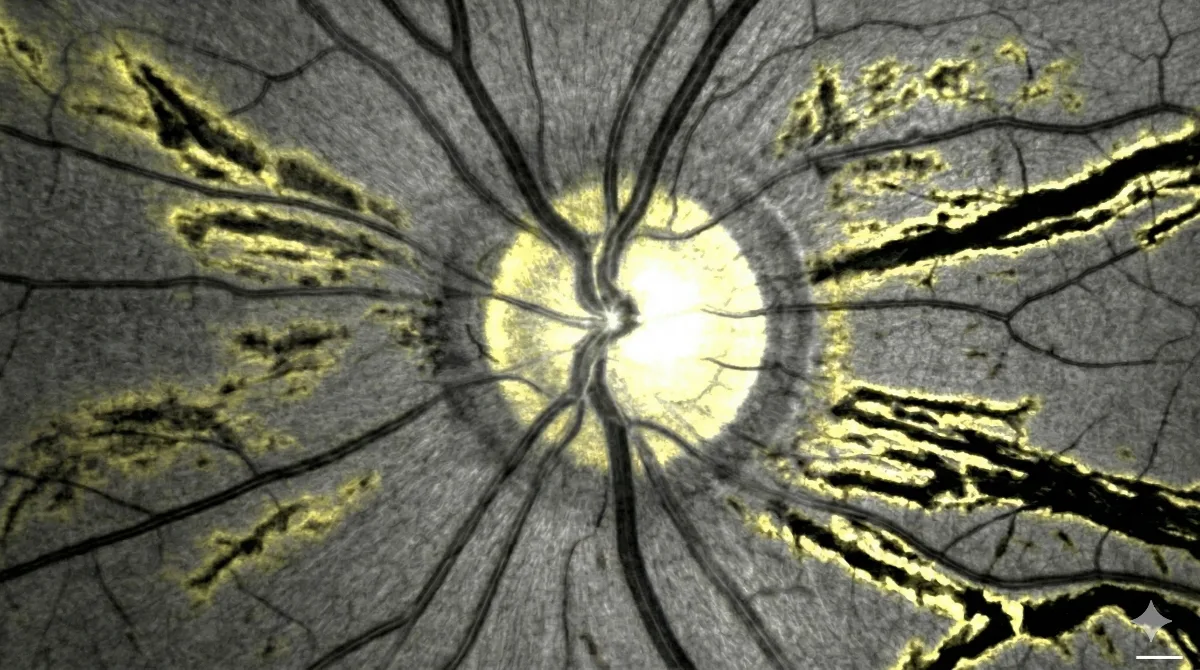
Angioid streaks are small cracks that appear in Bruch's membrane, a thin layer located beneath the retina. This membrane plays an essential role as it separates the retina from the choroid, the vascular tissue that nourishes the eye. When Bruch's membrane gradually calcifies, it becomes rigid and brittle. The natural mechanical stresses exerted on the eye then cause breaks that manifest as brownish, orange, or grayish lines radiating outward from the optic nerve.
Their name comes from their resemblance to blood vessels (angioid means "resembling a vessel"), although they are not vessels but actual cracks in this deep structure of the eye. Angioid streaks affect men and women equally and are most often discovered between the ages of 30 and 50, sometimes incidentally during a fundus examination.
Causes and diseases associated with angioid streaks
Angioid streaks may be isolated (so-called idiopathic forms) or occur in the context of a systemic disease. This is a fundamental point, as the discovery of angioid streaks should always prompt investigation for an underlying condition.
Pseudoxanthoma elasticum (PXE)
This is the most common and most important association to be aware of. Pseudoxanthoma elasticum is a rare genetic disease (mutation of the ABCC6 gene) that affects the elastic fibers throughout the body. It presents with characteristic skin signs (small yellowish papules on the neck and flexural creases), sometimes severe cardiovascular involvement (arteriopathy, hypertension, hemorrhages), and ocular lesions. Up to 85% of patients with PXE develop ocular signs, including angioid streaks. A dermatological, cardiological, and genetic workup is then essential.
Hemoglobinopathies
Sickle cell disease and thalassemias may also be associated with angioid streaks. In this context, serious ocular complications are somewhat less frequent, but monitoring remains necessary. A blood test (hemoglobin electrophoresis) can screen for these abnormalities.
Other associations
More rarely, angioid streaks are found in Paget's disease of bone, Marfan syndrome, Ehlers-Danlos syndrome, or other systemic conditions. Regardless of the cause, a complete etiological workup is systematically recommended.
Symptoms: when do angioid streaks become problematic?
In the vast majority of cases, angioid streaks are asymptomatic. They are often discovered incidentally during a routine ophthalmological examination. You may have angioid streaks for years without knowing it and without any visual impairment.
Symptoms arise in two situations:
- Extension toward the fovea: when a streak progresses to the central area of the retina (the fovea, responsible for fine vision), a decrease in visual acuity may occur.
- Choroidal neovascularization: this is the most feared complication. Abnormal new vessels develop through the breaks in Bruch's membrane and cause a macular syndrome: decreased vision, distortion of straight lines (metamorphopsia), or a dark spot in the center of the visual field (scotoma). This complication is comparable to that observed in wet AMD (age-related macular degeneration).
Any new visual symptom in a patient with angioid streaks constitutes an ophthalmological emergency requiring prompt consultation.
Diagnosis of angioid streaks: which examinations?
Diagnosis is based on a thorough fundus examination supplemented by high-precision retinal imaging studies. Dr Julien Gozlan has all the necessary equipment at the Paris – Auteuil Ophthalmology Practice.
- Fundus examination and retinal photography: angioid streaks appear as colored lines radiating from the optic nerve. Associated signs such as an "orange peel" appearance of the retina or optic disc drusen may be observed.
- Autofluorescence: this non-invasive examination makes angioid streaks more visible and allows monitoring of their progression as well as the advancement of any areas of retinal atrophy.
- OCT (optical coherence tomography): this is a key examination. OCT enables direct visualization of the breaks in Bruch's membrane, sometimes even before they are visible on fundus examination. It also detects signs of complications: serous retinal detachment, edema, and neovascularization.
- OCT angiography: this non-invasive examination maps the retinal and choroidal vessels without dye injection. It is particularly useful for detecting early or minimally active neovascularization, which can sometimes be difficult to identify with other techniques.
- Fluorescein angiography and indocyanine green angiography: these dye-based examinations remain valuable for assessing the activity of any neovascularization and guiding therapeutic decisions.
Treatment of angioid streaks and their complications
In the absence of complications, angioid streaks do not require specific treatment. Management then relies on regular monitoring and preventive measures.
Prevention and monitoring
Patients with angioid streaks should avoid ocular and facial trauma (combat sports, sports with a risk of impact). The weakened Bruch's membrane can indeed rupture further, even from an apparently minor impact, causing retinal hemorrhages. Daily self-monitoring with the Amsler grid (a simple test to detect visual distortions) is strongly recommended. Regular ophthalmological follow-up, at least annually, is essential.
Treatment of choroidal neovascularization
When neovascularization complicates angioid streaks, treatment relies on intravitreal injections (IVT) of anti-VEGF agents. These molecules (ranibizumab, aflibercept, bevacizumab) block the vascular growth factor responsible for the proliferation of abnormal new vessels. They are injected directly into the eye, painlessly under local anesthesia, during sessions performed in the office.
The advent of anti-VEGF agents has truly transformed the visual prognosis for patients. Before these treatments, neovascularization associated with angioid streaks almost inevitably led to severe visual impairment. Today, stabilization or even improvement of vision is achieved in 50 to 75% of cases, provided intervention is prompt and close follow-up is maintained. The first year often requires multiple injections and frequent check-ups to detect any recurrences.
It is important to note that, even with effective treatment, prolonged monitoring remains necessary. Some patients may develop long-term extension of retinal atrophy or fibrosis, requiring ongoing adjustment of their management.
Systemic management
When angioid streaks are associated with a systemic disease such as pseudoxanthoma elasticum, multidisciplinary management is organized. This involves consultations in dermatology, cardiology, and possibly hematology, in order to screen for and treat extra-ocular complications, particularly cardiovascular ones.
FAQ: angioid streaks
Are angioid streaks a serious condition?
Angioid streaks themselves are not dangerous as long as they remain stable and away from the center of the retina. However, they can be complicated by choroidal neovascularization threatening central vision. Furthermore, they are sometimes associated with serious systemic diseases. This is why ophthalmological follow-up and a systemic workup are essential.
Can angioid streaks be cured?
There is no treatment that can eliminate angioid streaks, as the breaks in Bruch's membrane are irreversible. However, neovascular complications are now very well managed thanks to intravitreal injections of anti-VEGF agents, which stabilize or even improve vision in the majority of cases.
Are intravitreal injections painful?
Intravitreal injections are performed under local anesthesia using anesthetic eye drops. The procedure is very quick (a few seconds) and generally painless. A brief sensation of discomfort or pressure may be felt, but the vast majority of patients tolerate this treatment very well. Dr Julien Gozlan ensures that each session takes place under the best conditions of comfort and safety.
How often should angioid streaks be monitored?
In the absence of complications, an annual ophthalmological check-up including OCT and fundus examination is recommended. If neovascularization is being treated, check-ups are much more frequent, particularly during the first year, with monthly or bimonthly examinations depending on progression. Daily self-monitoring with the Amsler grid is recommended.
Which sports should be avoided with angioid streaks?
All sports involving a risk of facial or ocular trauma should be avoided: combat sports (boxing, karate, judo), racquet sports with a risk of impact (squash), and more generally any activity exposing you to blows to the face. The weakened Bruch's membrane can rupture further even from a moderate impact, causing potentially serious retinal hemorrhages.
Do angioid streaks affect both eyes?
Yes, angioid streaks are most often bilateral, meaning they affect both eyes. However, the involvement is not necessarily symmetrical: one eye may be more affected than the other. Neovascular complications may also occur at different times in each eye, which is why regular monitoring of both eyes is important.
When to consult Dr Julien Gozlan?
Consult promptly if you have angioid streaks and notice a sudden decrease in vision, distortion of straight lines, a dark spot in the center of your visual field, or any other unusual visual symptom. These signs may indicate a neovascular complication requiring urgent treatment with intravitreal injections. If you have been diagnosed with pseudoxanthoma elasticum or a hemoglobinopathy and have never had a thorough fundus examination, a complete ophthalmological assessment with OCT and OCT angiography is strongly recommended to screen for possible angioid streaks and to organize appropriate follow-up.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan welcomes you at the Paris – Auteuil Ophthalmology Practice for the diagnosis, monitoring, and treatment of angioid streaks and their retinal complications. Equipped with the most advanced imaging technologies (OCT, OCT angiography, autofluorescence), he provides personalized and responsive care to best preserve your visual capital.
Book an Appointment on DoctolibFurther reading
- AMD: age-related macular degeneration: understand this common retinal disease that shares mechanisms with the complications of angioid streaks.
- Intravitreal injections (IVT): everything you need to know about the procedure, indications, and aftercare of this essential treatment for neovascularization.
- OCT: optical coherence tomography: discover this essential imaging examination for the diagnosis and monitoring of retinal diseases.
- OCT angiography: understand this non-invasive examination that is revolutionizing the detection of choroidal neovascularization.