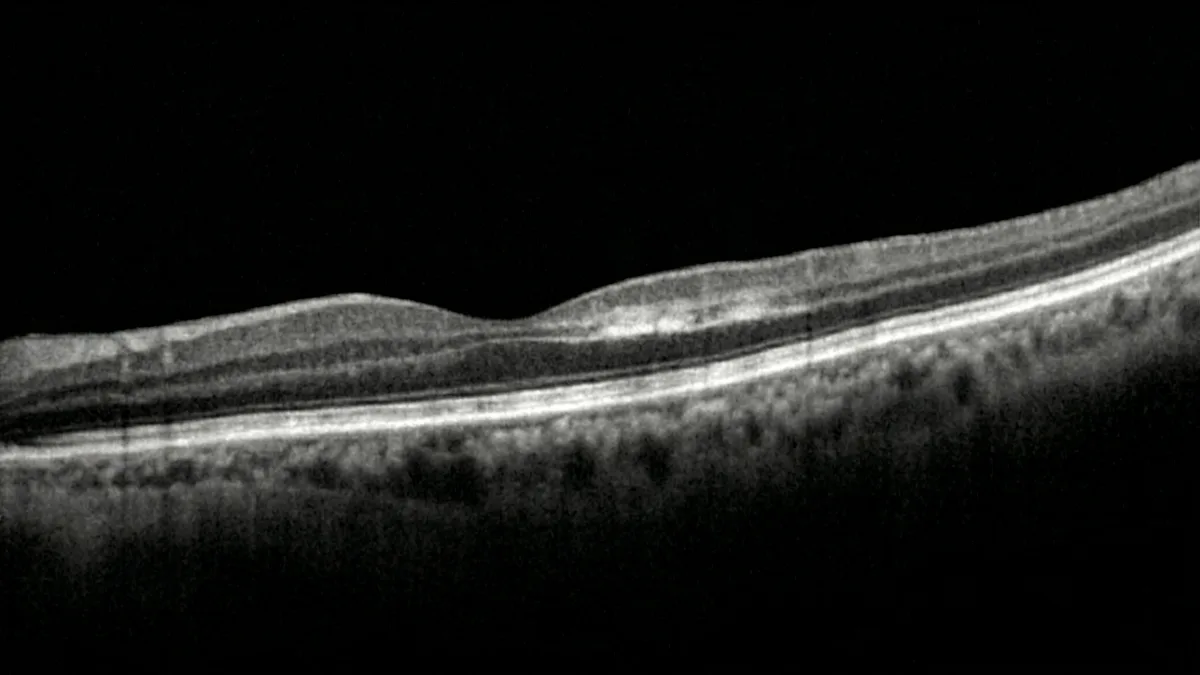
PAMM (Paracentral Acute Middle Maculopathy) is a recently identified ischemic retinal condition affecting the intermediate layers of the macular retina. Dr Julien Gozlan, ophthalmic surgeon specializing in retinal diseases and surgery in Paris 16, presents a comprehensive article on this still under-recognized condition. We will cover the precise definition of PAMM, its pathophysiological mechanisms, identified risk factors, characteristic symptoms, modern diagnostic modalities — particularly OCT and OCT angiography — as well as current management and long-term visual prognosis.
What is PAMM (Paracentral Acute Middle Maculopathy)?
PAMM was first described in 2013 by Sarraf and colleagues in the journal Retina. This entity corresponds to an acute ischemic event specifically affecting the intermediate layers of the retina, particularly the inner nuclear layer (INL) and the inner plexiform layer (IPL). Unlike classic retinal vascular occlusions that affect the superficial layers (branch retinal vein or artery occlusion), PAMM results from involvement of the deep capillary plexus of the macula.
From a vascular standpoint, the retina is supplied by two distinct capillary networks: the superficial plexus and the deep plexus. PAMM reflects selective ischemia of the deep plexus, which distinguishes it from other forms of retinal ischemia. This distinction has become possible thanks to advances in retinal imaging, particularly spectral domain OCT and OCT angiography, which enable layer-by-layer analysis of the retina with micrometric resolution.
Causes and risk factors of PAMM
The pathophysiology of PAMM is based on acute hypoperfusion of the deep macular capillary plexus. Several clinical contexts have been associated with this condition in the scientific literature (Rahimy et al., Retina, 2015; Chen et al., American Journal of Ophthalmology, 2015):
- Cardiovascular diseases: arterial hypertension, atherosclerosis, cardioembolic conditions, history of stroke.
- Retinal vasculopathies: PAMM may occur in isolation or be associated with a branch retinal artery occlusion (BRAO), central retinal artery occlusion, or advanced diabetic retinopathy.
- Prothrombotic states: coagulation disorders, sickle cell disease, antiphospholipid syndrome.
- Iatrogenic and toxic causes: some cases have been reported after use of vasoconstrictors, high-dose caffeine, or in a perioperative setting (cardiac surgery, prolonged general anesthesia).
- Retinal migraine: cases of PAMM have been described in migraine patients, suggesting a possible vasospastic mechanism.
- Idiopathic: in a number of cases, no etiology is identified, particularly in young subjects with no known cardiovascular risk factors.
It is important to emphasize that PAMM may constitute a warning sign revealing an underlying systemic vascular disease not yet diagnosed. A comprehensive cardiovascular workup is therefore recommended upon discovery of PAMM (Yu et al., Survey of Ophthalmology, 2018).
Symptoms and diagnosis of PAMM
Symptoms experienced by the patient
PAMM typically presents with the sudden onset of a paracentral scotoma, meaning a dark or grayish spot in the visual field, located near the fixation point but not directly affecting it in most cases. The patient often describes a blind or blurred area, fixed, that appeared within a few hours. Central visual acuity may be preserved or moderately decreased, which can sometimes make the initial clinical diagnosis difficult.
Fundus examination
On biomicroscopic fundus examination, PAMM can be very subtle or even invisible. A zone of subtle paracentral retinal whitening may sometimes be observed, but this abnormality is often difficult to detect without complementary imaging.
OCT: the key diagnostic examination
OCT (optical coherence tomography) is the essential examination to confirm the diagnosis of PAMM. The characteristic sign is a band-like hyperreflectivity at the level of the inner nuclear layer and inner plexiform layer of the retina, corresponding to ischemia and cytotoxic edema of the cells in these layers. At a later stage, this hyperreflectivity evolves toward thinning and atrophy of the inner nuclear layer, reflecting definitive cell loss (Sarraf et al., Retina, 2013).
OCT angiography: visualization of the deep plexus
OCT angiography (OCTA) represents a major advance in the understanding of PAMM. This non-invasive examination, without contrast dye injection, allows direct visualization of the decreased blood flow in the deep capillary plexus in the area corresponding to the scotoma. OCTA thus confirms the deep ischemic mechanism and helps differentiate PAMM from other macular conditions (Nemiroff et al., Retina, 2016).
Management and treatment of PAMM
To date, there is no validated specific treatment for PAMM. No randomized controlled trial has demonstrated the efficacy of a curative treatment. Management is based on several approaches:
- Systemic etiological workup: investigation of cardiovascular risk factors (lipid panel, blood glucose, blood pressure, coagulation tests, cardiac ultrasound, Doppler ultrasound of the supra-aortic trunks). This workup is essential because PAMM may reveal a silent vascular condition requiring urgent treatment.
- Treatment of the underlying cause: correction of cardiovascular risk factors, anticoagulation or antiplatelet therapy if indicated, management of any diabetes or arterial hypertension.
- Regular ophthalmological monitoring: follow-up with OCT and OCT angiography to track the progression of retinal lesions and detect any recurrence or contralateral involvement.
- No indication for intravitreal injections: unlike wet AMD treated with intravitreal anti-VEGF injections, PAMM does not warrant this type of treatment because the mechanism is ischemic, not neovascular.
Visual prognosis and progression of PAMM
The visual prognosis of PAMM varies depending on the extent and location of the ischemia. In limited forms, the paracentral scotoma may partially diminish over time, although a functional sequela often persists. The progressive atrophy of the inner nuclear layer, visible on OCT over the following weeks, reflects irreversible neuronal loss.
According to published series (Rahimy et al., 2015; Nakashima et al., BMC Ophthalmology, 2019), recovery of measured visual acuity is generally favorable when the fovea is spared. However, the residual paracentral scotoma can remain bothersome for reading and precision tasks. In forms associated with retinal artery occlusion, the prognosis depends on the overall extent of the ischemia.
PAMM may also recur, particularly in patients with uncontrolled vascular risk factors. Long-term monitoring is therefore recommended.
PAMM and differential diagnosis
The diagnosis of PAMM must be distinguished from several macular conditions that may present with similar symptoms:
- Acute Macular Neuroretinopathy (AMN): a closely related entity but affecting the outer retinal layers (outer nuclear layer), with different OCT findings.
- Branch retinal artery occlusion: ischemia of the superficial layers, with more visible retinal whitening on fundus examination.
- Epiretinal membrane: a different structural cause, clearly visible on OCT.
- Optic neuropathy: scotoma of neurological origin, without abnormalities of the inner retinal layers on OCT.
FAQ: PAMM — Frequently asked patient questions
Is PAMM an ophthalmic emergency?
The sudden onset of a scotoma (dark spot in the visual field) requires a prompt ophthalmological consultation, ideally within 24 to 48 hours. Although there is no specific emergency treatment for PAMM, an OCT examination is essential to establish the diagnosis. Furthermore, PAMM may be the revealing sign of a systemic vascular condition requiring urgent management.
Can PAMM cause permanent vision loss?
PAMM causes ischemia of the intermediate retinal layers that progresses to irreversible cell atrophy. The residual paracentral scotoma is often permanent, but central visual acuity is generally preserved if the fovea is not directly affected. The functional impact therefore varies from one patient to another depending on the location and extent of the lesion.
How is PAMM diagnosed?
The diagnosis is primarily based on OCT (optical coherence tomography), which shows characteristic hyperreflectivity of the intermediate retinal layers. OCT angiography completes the assessment by visualizing the decreased flow in the deep capillary plexus. Fundus examination alone may be insufficient because the abnormalities are often very subtle on direct observation.
Is there a treatment for PAMM?
There is currently no validated curative treatment for PAMM. Management consists of identifying and treating underlying vascular risk factors (hypertension, diabetes, coagulation disorders). Regular ophthalmological follow-up with OCT allows monitoring of retinal lesion progression. Research is ongoing to better understand this condition and identify potential therapeutic targets.
Can PAMM affect both eyes?
Although PAMM is most often unilateral, bilateral cases have been reported in the literature, particularly in patients with systemic vascular risk factors. Monitoring of the fellow eye is therefore recommended during follow-up. The comprehensive cardiovascular workup also aims to reduce the risk of involvement of the other eye.
PAMM and driving: are they compatible?
The presence of a paracentral scotoma can interfere with driving, particularly for detecting lateral obstacles and reading road signs. Compatibility with driving depends on the extent of the scotoma and residual visual acuity. A visual field examination and an evaluation by your ophthalmologist will determine whether driving remains safely permitted.
When to consult Dr Julien Gozlan?
Any sudden appearance of a dark spot, paracentral scotoma, or abrupt visual disturbance should prompt a rapid ophthalmological consultation. Dr Julien Gozlan, retinal disease specialist, has all the imaging equipment (spectral domain OCT, OCT angiography) required for accurate diagnosis of PAMM and other ischemic retinal conditions. If you have cardiovascular risk factors (diabetes, hypertension, vascular history), regular retinal monitoring is particularly recommended for early detection of any deep capillary plexus involvement.
📍 Consultation at the Paris – Auteuil Ophthalmology Practice
Dr Julien Gozlan welcomes you at the Paris – Auteuil Ophthalmology Practice for the diagnosis and follow-up of PAMM and all retinal diseases. With a state-of-the-art technical platform including OCT and OCT angiography, he supports you with rigor and compassion in the management of your visual health.
Book an appointment on DoctolibFurther reading
- OCT (optical coherence tomography): everything you need to know about this essential examination for retinal layer analysis.
- OCT angiography: principle and indications of retinal vascular imaging without injection.
- AMD: age-related macular degeneration: causes, diagnosis, and treatments of this common macular disease.
- Diabetic retinopathy: understanding diabetes-related retinal damage and its management.